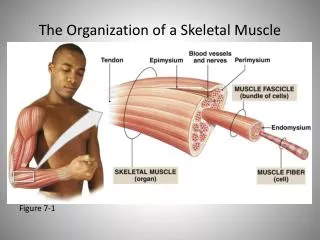
Skeletal Muscle: Structure and Function
Skeletal Muscle: Structure and Function. Objectives. Draw and label the microstructure of skeletal muscle. Define satellite cells. How do these cells differ from the nuclei located within skeletal muscle fibers? List the chain of events that occur during muscular contraction.


Skeletal Muscle: Structure and Function
E N D
Presentation Transcript
Objectives • Draw and label the microstructure of skeletal muscle. • Define satellite cells. How do these cells differ from the nuclei located within skeletal muscle fibers? • List the chain of events that occur during muscular contraction. • Define both dynamic and static exercise. What types of muscle action occur during each form of exercise?
Objectives • What three factors determine the amount of force produced during muscular contraction? • List the three human skeletal muscle fiber types. Compare and contrast the major biochemical and mechanical properties of each. • How does skeletal muscle fiber type influence athletic performance? • Graph and describe the relationship between movement velocity and the amount of force exerted during muscular contraction.
Structure of Skeletal Muscle Neuromuscular Junction Muscular Contraction Overview of the Sliding Filament Model Energy for Contraction Regulation of Excitation-Contraction Coupling Fiber Types Biochemical and Contractile Characteristics of Skeletal Muscle Characteristics of Individual Fiber Types Fiber Types and Performance Outline • Muscle Actions • Speed of Muscle Action and Relaxation • Force Regulation in Muscle • Force-Velocity/Force-Power Relationships • Alterations in Skeletal Muscle Due to Exercise, Inactivity, and Aging Exercise-Induced Changes in Skeletal Muscles Muscle Atrophy Due to Inactivity Age-Related Changes in Skeletal Muscle
Structure of Skeletal Muscle Skeletal Muscle • Human body contains over 400 skeletal muscles • 40-50% of total body weight • Functions of skeletal muscle • Force production for locomotion and breathing • Force production for postural support • Heat production during cold stress • Muscle actions • Flexors • Decrease joint angle • Extensors • Increase joint angles
Structure of Skeletal Muscle Connective Tissue Covering Skeletal Muscle • Epimysium • Surrounds entire muscle • Perimysium • Surrounds bundles of muscle fibers • Fascicles • Endomysium • Surrounds individual muscle fibers • External lamina • Just below endomysium • Sarcolemma • Muscle cell membrane
Structure of Skeletal Muscle Connective Tissue Surrounding Skeletal Muscle Figure 8.1
Structure of Skeletal Muscle Satellite Cells • Play role in muscle growth and repair • Increase number of nuclei • Myonuclear domain • Cytoplasm surrounding each nucleus • Each nucleus can support a limited myonuclear domain • More nuclei allow for greater protein synthesis • Important for adaptations to strength training
Structure of Skeletal Muscle Microstructure of Muscle Fibers • Myofibrils • Contain contractile proteins • Actin (thin filament) • Myosin (thick filament) • Sarcomere • Includes Z line, M line, H zone, A band, I band • Sarcoplasmic reticulum • Storage sites for calcium • Terminal cisternae • Transverse tubules • Extend from sarcolemma to sarcoplasmic reticulum
Structure of Skeletal Muscle Microstructure of Skeletal Muscle Figure 8.2
Structure of Skeletal Muscle The Sarcoplasmic Reticulum and Transverse Tubules Figure 8.3
Neuromuscular Junction Neuromuscular Junction • Junction between motor neuron and muscle fiber • Motor unit • Motor neuron and all fibers it innervates • Motor end plate • Pocket formed around motor neuron by sarcolemma • Neuromuscular cleft • Short gap between neuron and muscle fiber • Acetylcholine is released from the motor neuron • Causes an end-plate potential (EPP) • Depolarization of muscle fiber
Neuromuscular Junction The Neuromuscular Junction Figure 8.4
Neuromuscular Junction In Summary • The human body contains over 400 voluntary skeletal muscles, which constitute 40% to 50% of the total body weight. Skeletal muscle performs three major functions: (1) force production for locomotion and breathing, (2) force production for postural support, and (3) heat production during cold stress. • Individual muscle fibers are composed of hundreds of threadlike protein filaments called myofibrils. Myofibrils contain two major types of contractile protein: (1) actin (part of the thin filaments) and (2) myosin (major component of the thick filaments).
Neuromuscular Junction In Summary • The region of cytoplasm surrounding an individual nucleus is termed the myonuclear domain. The importance of the myonuclear domain is that a single nucleus is responsible for the gene expression for its surrounding cytoplasm. • Motor neurons extend outward from the spinal cord and innervate individual muscle fibers. The site where the motor neuron and muscle cell meet is called the neuromuscular junction. Acetylcholine is the neurotransmitter that stimulates the muscle fiber to depolarize, which is the signal to start the contractile process.
Muscular Contraction The Sliding Filament Model • Muscle shortening occurs due to the movement of the actin filament over the myosin filament • Formation of cross-bridges between actin and myosin filaments • Power stroke • Reduction in the distance between Z lines of the sarcomere
Muscular Contraction The Sliding Filament Theory of Contraction Figure 8.5
Muscular Contraction The Relationships Among Troponin, Tropomyosin, Myosin, and Calcium Figure 8.6
Muscular Contraction Energy for Muscle Contraction • ATP is required for muscle contraction • Myosin ATPase breaks down ATP as fiber contracts • ATP ADP + Pi • Sources of ATP • Phosphocreatine (PC) • Glycolysis • Oxidative phosphorylation
Muscular Contraction Sources of ATP for Muscle Contraction Figure 8.7
Muscular Contraction A Closer Look 8.1Muscle Fatigue • Decrease in muscle force production • Reduced ability to perform work • Contributing factors: • High-intensity exercise (~60 seconds) • Accumulation of lactate, H+, ADP, Pi, and free radicals • Long-duration exercise (2–4 hours) • Muscle factors • Accumulation of free radicals • Electrolyte imbalance • Glycogen depletion • Central fatigue • Reduced motor drive to muscle from CNS
Muscular Contraction Muscular Fatigue Figure 8.8
Muscular Contraction Excitation-Contraction Coupling • Depolarization of motor end plate (excitation) is coupled to muscular contraction • Action potential travels down transverse tubules and causes release of Ca+2 from SR • Ca+2 binds to troponin and causes position change in tropomyosin • Exposing active sites on actin • Strong binding state formed between actin and myosin • Contraction occurs
Muscular Contraction A Closer Look 8.2Step-by-Step Summary of Excitation-Contraction Coupling • Excitation • Action potential in motor neuron causes release of acetylcholine into synaptic cleft. • Acetylcholine binds to receptors on motor end plate, leads to depolarization that is conducted down transverse tubules, which causes release of Ca+2 from sarcoplasmic reticulum (SR).
Muscular Contraction A Closer Look 8.2Step-by-Step Summary of Excitation-Contraction Coupling • Contraction • At rest, myosin cross-bridges in weak binding state. • Ca+2 binds to troponin, causes shift in tropomyosin to uncover active sites, and cross-bridge forms strong binding state. • Pi released from myosin, cross-bridge movement occurs. • ADP released from myosin. • ATP attaches to myosin, breaking the cross-bridge and forming weak binding state. Then ATP binds to myosin, broken down to ADP+Pi, which energizes myosin. Continues as long as Ca+2 and ATP are present.
Muscular Contraction Muscle Excitation, Contraction, and Relaxation Figure 8.9
Muscular Contraction Steps Leading to Muscular Contraction Figure 8.10
Muscular Contraction In Summary • The process of muscular contraction can be best explained by the sliding filament model, which proposes that muscle shortening occurs due to movement of the actin filament over the myosin filament. • The steps in muscular contraction are: • The nerve impulse travels down the transverse tubules and reaches the sarcoplasmic reticulum, and Ca+2 is released. • Ca+2 binds to the protein troponin. • Ca+2 binding to troponin causes a position change in tropomyosin away from the “active sites” on the actin molecule and permits a strong binding state between actin and myosin. • Muscular contraction occurs by multiple cycles of cross-bridge activity. Shortening will continue as long as energy is available and Ca+2 is free to bind to troponin.
Muscular Contraction In Summary • When neural activity ceases at the neuromuscular junction, Ca+2 is removed from the sarcoplasmic reticulum by the Ca+2 pump. This results in tropomyosin moving to cover the active site on actin, and the muscle relaxes.
Fiber Types Characteristics of Muscle Fiber Types • Biochemical properties • Oxidative capacity • Number of capillaries, mitochondria, and amount of myoglobin • Type of myosin ATPase • Speed of ATP degradation • Contractile properties • Maximal force production • Force per unit of cross-sectional area • Speed of contraction (Vmax) • Myosin ATPase activity • Muscle fiber efficiency
Fiber Types A Closer Look 8.3How Are Muscle Fibers Typed? • Muscle biopsy • Small piece of muscle removed • May not be representative of entire body • Staining for type of myosin ATPase • Type I fibers appear darkest • IIa fibers lightest • IIx fibers in between • Immunohistochemical staining • Selective antibody binds to unique myosin proteins • Fiber types differentiated by color difference • Gel electrophoresis • Identify myosin isoforms specific to different fiber types
Fiber Types Immunohistochemical Staining of Skeletal Muscle Blue = Type I fibers Green = Type IIa fibers Black = Type IIx fibers Red = dystrophin (protein in sarcolemma) Figure 8.11
Fiber Types Characteristics of Individual Fiber Types • Type IIx fibers • Fast-twitch fibers • Fast-glycolytic fibers • Type IIa fibers • Intermediate fibers • Fast-oxidative glycolytic fibers • Type I fibers • Slow-twitch fibers • Slow-oxidative fibers
Fiber Types Characteristics of Muscle Fiber Types
Fiber Types Comparison of Maximal Shortening Velocities Between Fiber Types Figure 8.12
Fiber Types A Closer Look 8.4Do Fast Fibers Exert More Force Than Slow Fibers? • Maximal force per cross-sectional area • 10–20% higher in fast fibers (IIa and IIx) compared to slow (Type I) fibers • Force production related to number of myosin cross-bridges in strong binding state • Fast fibers contain more cross-bridges per cross-sectional area
Fiber Types In Summary • Human skeletal muscle fiber types can be divided into three general classes of fibers based on their biochemical and contractile properties properties. Two categories of fast fibers exist, type IIx and type IIa. One type of slow slow fiber exists, type I fibers. • The biochemical and contractile properties characteristic of all muscle fiber types are summarized in table 8.1.
Fiber Types In Summary • Although classifying skeletal muscle fibers into three general groups is a convenient system to study the properties of muscle fibers, it is important to appreciate that human skeletal muscle fibers exhibit a wide range of contractile and biochemical properties. That is, the biochemical and contractile properties of type IIx, type IIa, and type I fibers represent a continuum instead of three neat packages.
Fiber Types Fiber Types and Performance • Nonathletes • Have approximately 50% slow and 50% fast fibers • Power athletes • Sprinters • Higher percentage of fast fibers • Endurance athletes • Distance runners • Higher percentage of slow fibers • Fiber type is not the only variable that determines success in an athletic event
Fiber Types Distribution of Fiber Type in Athletes
Fiber Types In Summary • Successful power athletes (e.g., sprinters) generally possess a large percentage of fast muscle fibers and, therefore, a low percentage of slow, type I fibers. • In contrast to power athletes, endurance athletes (e.g., marathoners) typically possess a high percentage of slow muscle fibers and a low percentage of fast fibers.
Alterations in Skeletal Muscle Due to Exercise, Inactivity, and Aging Exercise-Induced Changes in Skeletal Muscles • Strength training • Increase in muscle fiber size (hypertrophy) • Increase in muscle fiber number (hyperplasia) • Limited evidence in humans • Endurance training • Increase in oxidative capacity • Alteration in fiber type with training • Fast-to-slow shift • Type IIx IIa • Type IIa I with further training • Seen with endurance and resistance training
Alterations in Skeletal Muscle Due to Exercise, Inactivity, and Aging Effects of Endurance Training on Fiber Type Figure 8.13
Alterations in Skeletal Muscle Due to Exercise, Inactivity, and Aging Muscle Atrophy Due to Inactivity • Loss of muscle mass and strength • Due to prolonged bed rest, limb immobilization, reduced loading during space flight • Initial atrophy (2 days) • Due to decreased protein synthesis • Further atrophy • Due to reduced protein synthesis • Atrophy is not permanent • Can be reversed by resistance training • During spaceflight, atrophy can be prevented by resistance exercise
Alterations in Skeletal Muscle Due to Exercise, Inactivity, and Aging Age-Related Changes in Skeletal Muscle • Aging is associated with a loss of muscle mass • 10% muscle mass lost between age 25–50 years • Additional 40% lost between age 50–80 years • Also a loss of fast fibers and gain in slow fibers • Also due to reduced physical activity • Regular exercise training can improve strength and endurance • Cannot completely eliminate the age-related loss in muscle mass
Alterations in Skeletal Muscle Due to Exercise, Inactivity, and Aging In Summary • Both endurance and resistance exercise training have been shown to promote a fast-to-slow shift in skeletal muscle fiber types. However, this exercise-induced shift in fiber type is typically small and does not result in a complete transformation of all fast fibers (type II) into slow fibers (type I). • Prolonged periods of muscle disuse (bed rest, limb immobilization, etc.) result in muscle atrophy. This inactivity-induced atrophy results in a loss of muscle protein due to a reduction in protein synthesis and an increase in the rate of muscle protein breakdown.
Alterations in Skeletal Muscle Due to Exercise, Inactivity, and Aging In Summary • Aging is associated with a loss of muscle mass. This age-related loss of muscle mass is low from age 25 to 50 years but increases rapidly after 50 years of age. • Regular exercise training can improve skeletal muscle strength and endurance in the elderly but cannot completely eliminate the age-related loss of muscle mass.
Muscle Actions Types of Muscle Action • Isometric • Muscle exerts force without changing length • Pulling against immovable object • Postural muscles • Isotonic (dynamic) • Concentric • Muscle shortens during force production • Eccentric • Muscle produces force but length increases
Muscle Actions Muscle Actions
Muscle Actions Isometric and Isotonic Muscle Actions Figure 8.14