NOISE
NOISE. “Unnecessary noise, then, is the most cruel absence of care which can be inflicted either on sick or well.”. By Ameya Nerurkar Mandar Samant Chih-Pin Hsiao. By Florence Nightingale, 1859. Causes Of Noise. Standards and Current Conditions.


NOISE
E N D
Presentation Transcript
NOISE “Unnecessary noise, then, is the most cruel absence of care which can be inflicted either on sick or well.” By Ameya Nerurkar Mandar Samant Chih-Pin Hsiao By Florence Nightingale, 1859
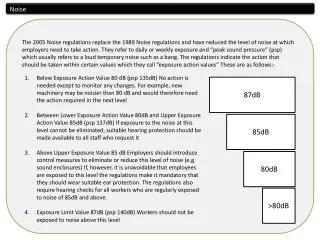
Standards and Current Conditions In 1995, Guidelines for Community Noise from World Health Organization (WHO) recommends an Lmax of no more than 40 dB(A) at night measure on the fast setting. They also suggest patient room Leq of no more than 35dB(A) during the day and 30 dB(A) at night. Study shows that the average day time sound levels in Johns Hopkins Hospitals are 72 dB(A). The typical speech level for communication between two people is 45-50 dB(A)
Effects Of Noise • Several adverse effects are associated with noise • increase noradrenalin concentrations in urine, hypertension and myocardial infarction • Sleep disturbance • exposure to sudden, unexpected noise raises patient heart rates • tend to increase blood pressure levels • In a hospital environment, where people are already ill and psychologically stressed, unnecessary noise can be very harmful • Could cause staff stress and burnout
Solutions Assessing and managing Sound Environment Identify Sources of noise Maintenance and replacement of Hospital equipments Layout and acoustic treatment of patients’ rooms and corridors etc Equipment Repair and Replacement Scheduling regular maintenance to keep equipments in working order padding chart holders and pneumatic tube systems, and lowering volume levels on clinical and communication equipment purchasing choices that are based on auditory performance Design of Patient rooms and adjacent Areas: Standardize on single bed private room
Results • Noise levels ranged between 49 and 89 dB (A) with a mean of 65 dB (A). • Peak noise levels were measured as high as 89 dB (A). • The noise levels measured at different locations in the intensive care unit did not differ significantly. • Noises created by other patients, those who were admitted from emergency room and operating room into intensive care unit, monitor alarms, conversations among staff were the most disturbing noise sources for patients.
Conclusions • The patients who were located in the bed which was closer to the nurses' station were more affected by the intensive care unit noise than other patients. • Having a previous intensive care unit experience also affected the patients' disturbance levels owing to noise. • Relevance to clinical practice: Nurses are in key positions where they can identify physical, psychological and social stressors that affect patients during their hospital stay. Staff education, planned nursing activities and proper design of intensive care unit may help combat this overlooked problem.
ICU Admission and Transfer/Discharge GuidelinesSt. Joseph Hospital 2009 ICU Admission and Discharge Criteria Mengdie Hu, Karsten M. Jensen, Thomas Roh • A list of criteria for the admission to ICU • Made to assure the appropriate utilization and resources of the ICU
Analysis of indications for early discharge from the intensive care unit Bone et al. 1993 • Patients with moderately severe illness benefit more from ICUs than patients who are severely ill or not very ill. • A predictive model can be developed to determine the mortality risk 24h after admission.
Consequences of discharges from intensive care at nightGoldfred et al. 2000 • Patients who are discharged at night have a much higher risk of dying • Night discharges are more likely to be premature • Insufficiency of intensive-care beds
Critically ill patients readmitted to intensive care units--lessons to learn?Metnitz et al. 2003 • Readmission raises the risk of dying more than four times • Residual organ dysfunctions at time of discharge • Optimizing organ functions in patients before discharge
Triaging patients to the ICU: a pilot study of factors influencing admission decisions and patient outcomesGarrouste-Orgeas et al. 2003 • Patients triaged by a senior physician are more likely to be refused admission • Refusal are related to patient age, underlying diseases, self-sufficiency and number of beds available
The patient-at-risk team (PART): identifying and managing seriously ill ward patientsGoldhill et al. 1999 • Patients admitted from hospital wards to ICU have a higher mortality then patients admitted from other areas • The PART protocol are a simple way of trying to identify critically ill patients on wards
Analysis of indications for early discharge from the intensive care unit.Bone et. al 1993 • Measures: Mortality and Quality of Life • Acute Physiology and Chronic Health Evaluation (APACHE) • Objective methods for determining patient discharge from ICU
Mortality among appropriately referred patients refused admission to intensive-care unitsMetcalfe et al. 1997 • UK - excess mortality for those too ill or too well • 9% higher rate of mortality • More ICU beds or better admission and discharge criteria
Guideline on Admission and Discharge for Adult Intermediate Care UnitsAmerican College of Critical Care Medicineof the Society of Critical Care Medicine 1998 • Admit low risk patients to intermediate care units • List of Requirements • Labor cost reduction
Discharge Criteria - A new trendChung 1995 • Discharging patients after anesthesia and surgery • Mathematical scoring system for five different areas • Recommends using a numerical system to determine discharging a patient