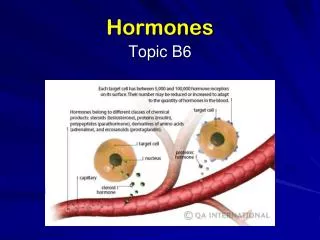
A. Thyroids Hormones
A. Thyroids Hormones. Iodide : actively transported into the thyroid follicular cell -> Thyroid peroxide (TPO) oxidizes iodide near the cell-colloid surface & Incorporates it into tyrosyl residues within the thyroglobulin molecule

A. Thyroids Hormones
E N D
Presentation Transcript
A. Thyroids Hormones Iodide : actively transported into the thyroid follicular cell -> Thyroid peroxide (TPO) oxidizes iodide near the cell-colloid surface & Incorporates it into tyrosyl residues within the thyroglobulin molecule result in the formation of monoiodotyrosine (MIT) & diiodotyrosine (DIT) Triiodothyronine (T3) & Thyroxine (T4) formed by secondary coupling of MIT & DIT catalyzed by TPO
TPO : membrane-bound, heme-containing oligomer, localized in rourg ER, Golgi vesicle & follicular cell surface • Thyroid antimicrosomal antibodies found in patients with autoimmune thyroid disease are directed against the TPO enzyme • Thyroid-stimulating hormone (TSH) : regulates thyroidal iodine metabolism by activation of adenylate cyclase --> facilitates endocytosis, digestion of thyroglobulin-containing colloid & release of thyroid hormones T4, T3, rT3 • Thyroid hormones - effects on cells include increased oxygen consumption, heat production, increased metabolism of fat, proteins & carbohydrate
1. Iodide Metabolism - Daily allowance : 150 ~ 300 g/day - Sufficiency of iodine : associated with development of autoimmune thyroid disorder. 2. Factors affecting Thyroid function - Iodide - Pollutants (plasticizers, polychlorinated bipheols & coal processing pollutants) - Ab to Yersinia enterocolitica. • Female hormonal milieu & its potential effects on immune surveillance
B. Evaluation 1. Thyroid Function. ↑TBG conditions : pregnancy, oral pill, ERT, hepatitis, genetic abnormality of TBG, --> require measuring T3RU for clarification. FTI ( Free T4 Index ) : % free T4 ( T3RU ) × T4 total TSH measurement : best single screen for thyroid dysfunction.
2. Immunologic Abnormalities -Antithyroglobuliin Ab. : noncomplement-fixing IgG polyclonal antibodies, (+) in Hashimoto's thyroiditis, Graves' Dz, acute thyroiditis, nontoxic goiter, thyroid cancer, normal women. -Antimicrosomal antibody-direct against TPO : cytotoxic, complement fixing Ig G Ab (+) in Hashimoto's thyroiditis, Graves' disease & postpartum thyroiditis
-Atibody to T3 & T4. : (+) in Hashimoto's thyroiditis & Graves' Dz. who have antithyroglobulin Antibody -Antibody to TSH receptor -TSAb. (Thyroid-stimulating Ab) or TSI (Thyroid stimulating Ig) : monoclonal or limited polyclonal --> mimic TSH action -TBII (TSH-binding Inhibitor Ig) -block TSH binding -block both pre-& postreceptor process -TGI (Thyroid Growth-promoting Ig) • - stimulate growth, but not hormone release.
C. Autoimmune Thyroid Disease -Hypothyroidism > hyperthyroidism -F>M -Other autoimmune conditions associated with Graves' Dz. : Hashimoto's thyroiditis, Addison's Dz, ovarian failure, RA, Sjoren's SD, IDDM, vitiligo, pernicious anemia, MG, ITP...
1. Hashimoto's thyroiditis - Chronic lymphocytic thyroiditis - Present as hyperthyroidism, hypothyroidism, euthyroid goiter, or diffuse goiter. - High levels of anti-microsomal & antithyroglobulin Ab (+) - The composition of various Ab (TBII, TGI etc.) result in varied physical finding - Autoantibody TBII : causing the atophic form & congenital hypothyroidism in some neonates. TGI : causing the goitrous variety - 3 Classic types of autoimmune injury complement-mediated cytotoxicity Ab dependant cell mediated cytotoxicity stimulation or blockade of hormone receptor
1) Clinical Characteristics & Dx. - Mostly, relatively asymptomatic with painless goiter & hypothyroidism - Symptom : Cold intolerance, constipation, carotene deposition in the periorbital region, carpal tunnel syndrome, dry skin, fatigue, hair loss, lethargy, wt.gain. c.f Hashitoxicosis (<-- represent a variant of Graves' Dz.) - in 4~8% -Diagnosis ↑ TSH level during routine screening ↑ serum antithyroglobulin & antimicrosomal Ab ↑ ESR
2) Treatment Symptomatic hypothyroidism T4 replacement Goiter Can’t regress the size but prevent further growth of size Pregnant women with↑ TSH level • L-thyroxine. :Can’t slow progression of the disease 6wks of Tx are necessary before the effect of the dose change
2. Reproductive effects of Hypothyroidism . - Hypothyroidism : a/w↓ fertility resulting from ovulatory difficulties and not spontaneous abortion. - Menorrhagia, amenorrhea, anovulation, luteal phase defect • TSH increase defective in Dopamine turnover Enhanced sensitivity of prolactin secreting cell hyperprolactinemia - Replacement therapy - reverse the hyperprolactinemia & correct ovulatory defect
3. Graves' Disease Heritable specific defect by suppressor T cell development of helper T cell react to thyroid antigen induce B-cell mediated response Result in the clinical feature of Graves’ dz HLA class II antigen DR, DP, DQ, DS can present antigen to T cell
1) Clinical Characteristics & Dx. Classical triad : Exophthalmos, goiter, & hyperthyroidism symptom :↑bowel movement, heat intolerance, irritability, nervousness, palpitation, tachycardia, tremor, wt.loss, lower external swelling. P/E : lidlag, nontender thyroid enlargement, onycholysis, palmar erythema, proptosis, staring gaze, thick skin... if. severe cases : acropachy, chemosis, clubbing, dermopathy, exophalmus with ophthalmoplegia, follicular conjunctivitis, pretibial myxedema, vision loss.
Diagnosis T3 ↑, but T4 levels - mostly normal TSH↓ Antimicrosomal Ab (+) TSAb : useful in evaluating medical treatment, prognosis & potential fetal complication..
2) Treatment Medication --> potentially harmful effects on the fetus, special attention must be given to the case of contraception & the potential for pregnancy. (1) 131I Ablation Effective care in about 80% of cases Most commonly utilized definitive Tx. in nonpregnant women Postablative hypothyroidism : 50% within 1st year. (2) Antithyroid Drugs (3) Surgery (4) β-blocker
* Antithyroid Drugs • PTU & Methimazole Low doses : block the secondary coupling Rx. that form T3 & T4 from DIT & MIT. Higher doses --> block iodination of tyrosyl residues in thyroglobulin. 30% --> remission. 2. PTU (100mg, every 8 ~ 24hr) - block the intrathyroid synthesis of T3 & the pph conversion of T4 to T3. - not cross placenta. • drug of choice in pregnancy. 3. Methimazole (10mg, every 8 ~ 24hr) - not drug of choice in pregnancy , d/t not block pph conversion & cross placenta. 4. Iodide & Lithium. • reduce thyroid hormone release & inhibit the organification of iodine.
* Surgery Subtotal thyroidectomy Ix. Medical Tx failed Hypersensitive to medical Tx. Risk Hypoparathyroidism Recurrent laryngeal n. paralysis Hypothyroidism.
4. Reproductive Effects of Hyperthyroidism • Most women. : ovulatory & fertile • Severe thyrotoxicosis : wt. loss, irregular mens, amenorrhea, ↑spontaneous abortion, ↑congenital anomalies.
5. Postpartum Thyroid Dysfunction • Often difficult to diagnose, • Sx. appear 1 ~ 8 months postpartum. • Incidence : 5 % -> 25% permanent hypothyroid • Histo : lymphocytic infiltration & inflammation. • Antimicrosomal Ab (+)
1) Clinical Characteristics & Dx. Symptom : Depression, fatigue, palpitation, at 6 ~ 12 wks. postpartum. c.f. postpartum thyroid dysfunction should be considered in all women with postpartum psychosis. Diagnosis : (-) of thyroid tenderness, pain, fever, ↑ESR, leucocytosis TSH, T4, T, T3RU, antimicrosomal Ab titer. 2) Treatment : mostly hypothyroid phase and require 6 ~ 12 months of T4 replacement if they are symptomatic. (c.f.. 10 ~ 30% --> permanent hypothyroidism) : rarely hyperthyroid phase : not routinely use of anti-thyroid medication, but propranolol for symptomatic relief.