Acute Renal Failure
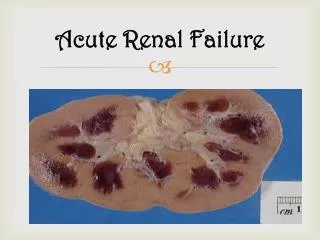
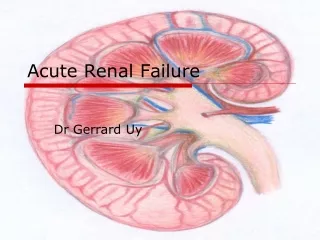
Acute Renal Failure. Terry Cook Imperial College London. Acute Renal Failure. Rapid loss of glomerular filtration and tubular function leading to abnormal water, electrolyte and solute balance Occurs over hours to days

Acute Renal Failure
E N D
Presentation Transcript
Acute Renal Failure Terry Cook Imperial College London
Acute Renal Failure • Rapid loss of glomerular filtration and tubular function leading to abnormal water, electrolyte and solute balance • Occurs over hours to days • Usually associated with oliguria. Some patients develop non-oliguric ARF eg. After radiocontrast media • Acute-on chronic renal failure
Aetiology of ARF • Pre-renal • Renal • Glomerular • Tubulointerstitial • Vascular • Post-renal
Aetiology of ARF • Glomerular • RPGN • Tubulointerstitial • Acute tubular necrosis • Acute tubulointerstitial nephritis • Infection • Cast nephropathy • Vascular • Thrombotic microangiopathy • Cholesterol emboli • Vasculitis
Rapidly Progressive Glomerulonephritis (RPGN) • RPGN is a clinical term for clinical manifestations that suggest severe crescentic glomerulonephritis • Crescentic glomerulonephritis – may be used for glomerulonephritis with any crescents but WHO suggests >50%
Crescentic glomerulonephritis • Crescents are an indication of severity of glomerulonephritis rather than its cause • Complete pathological diagnosis requires analysis of immunofluorescence, electron microscopy and serology
Natural history of crescents Breach in integrity of GBM – ROS, proteases etc from inflammatory cells Cells and fibrin in Bowman’s space Accumulation of macrophages and proliferating epithelial cells Apoptosis of cells and laying down of collagen Fibrocellular crescents and fibrous crescents
Causes of crescentic glomerulonephritis • Anti-GBM disease • Immune complex disease • Pauci-immune
Frequency of types of crescentic GN After Jenette and Falk
Anti-GBM disease • Presents with RPGN often accompanied by lung haemorrhage • Rare disorder (1 pmp) predominantly in Caucasian populations • Characterised by circulating and deposited anti-GBM antibodies
Pauci-immune crescentic GN • Basic lesion is focal and segmental necrosis • Often associated with vasculitis either in kidney or elsewhere
Pauci-immune crescentic GN - syndromes • Limited to kidney • Microscopic polyangiitis – necrotizing vasculitis in other systems including skin, mucous membranes, lungs, brain, gastrointestinal tract and muscle • Wegener’s granulomatosis – similar lesions to microscopic polyangiitis together with necrotizing granulomas of the upper and lower respiratory tract • Churg-Strauss syndrome – history of asthma or allergic rhinitis and blood eosinophilia N.B. These syndromes cannot be distinguished on the basis of renal histology
ANCA in small vessel vasculitis IIF pattern: C-ANCA P-ANCA Antigen: Proteinase 3 Myeloperoxidase Syndromes: WG,MP MP, renal-limited vasculitis
Clinical studies of ANCA • Specific and sensitive marker for systemic vasculitis • ANCA pattern and specificity correlate with clinical features • Levels correlate with disease activity and extent • Rising levels predict relapse
European Vasculitis Study Group biopsy findings • Biopsies from 96 patients with ANCA-associated vasculitis and creatinine <500 mmol/l • Studied • GFR0 – GFR at presentation • GFR18 – GFR at 18 months • CORGFR18 – GFR at 18 months corrected for GFR0
European Vasculitis Study Group biopsy findings • Predictors for GFR0 • %normal glomeruli • %glomeruli with crescents • Extent of tubular atrophy and interstitial fibrosis
European Vasculitis Study Group biopsy findings • Predictors for CORGFR18 • % glomeruli with fibrinoid necrosis • % glomeruli with cellular crescents • Tubulointerstitial inflammation • Tubular atrophy and interstitial fibrosis did not predict CORGFR18 even though they correlated with GFR18 implying that this was dependent on GFR0
European Vasculitis Study Group biopsy findings • In ANCA GN the best histological predictors of long-term renal function are • Normal glomeruli, glomerulosclerosis, interstitial fibrosis and tubular atrophy • The best predictors of the improvement in renal function from 0 to 18 months are • Crescents, fibrinoid necrosis and interstitial inflammation
Acute tubular necrosis • Prolonged hypoperfusion • Drugs – NSAIDs, ACE inhibitors • Direct toxicity • Drugs – eg. Aminoglycosides, cisplatin • Radiocontrast agents • Haem pigments • Snake venom • Heavy metals – lead , mercury • Associated with nephrotic syndrome
Acute tubular necrosis Tubular dilatation Loss of brush border Epithelial cell vacuolation Detachment of epithelial cells Granular casts Hyperchromasia of tubular nuclei Mitoses Calcification Interstitial oedema Interstitial inflammation Nucleated rbcs in vasa recta
Acute tubulointerstitial nephritis • Infectious eg. HIV, BKV, fungi, TB • Drugs • Post infectious • SLE • ANCA associated • With uveitis (TINU)
Acute tubulointerstitial nephritis • Interstitial infiltrate of mononuclear cells • Mainly T cells and macrophages • Tubulitis • +/- eosinophils • May rarely be anti-TBM antibodies
Granulomatous tubulointerstitial nephritis • Infectious • Sarcoidosis • Drugs • Idiopathic
Myeloma Cast Nephropathy • Light chains precipitate in tubules • Casts are large and eosinophilic – may be fractured or fragemented • Multinucleate giant cells my be found adjacent to casts • In some cases the casts may stain for amyloid • Interstitium typically shows an infiltrate of lymphocytes and macrophages
Thrombotic microangiopathy • Haemolytic-uraemic syndrome • Infection – particularly verotoxin-producing E. coli • Drugs – CNIs, mitomycin • Transplant rejection • Antiphospholipid antibodies • Post-partum • Factor H deficiency • Bone marrow transplantation • Thrombotic thrombocytopenic pupura • Malignant Hypertension • Scleroderma
Thrombotic microangiopathy • Glomeruli • Thrombosis • Trapped fragmented rbc • Thickened capillary walls with subendothelial fibrin • Ischaemic changes • Arterioles – fibrinoid • Interlobular arteries – loose intimal thickening
Cholesterol emboli • Common cause of unexplained renal failure in elderly • Predisposing factors • Trauma eg catheterisation, surgery • Anticoagulation • Spontaneous • May be slowly progressive • May involve glomeruli