Head Injuries
Head Injuries. 1,000,000 Pt’s / yr in A&E 6000 severe – 40-50% die Biggest killer for 15-24’s. Head Injuries. Skin Skull Meninges Brain Brain sits in CSF fluid (acts as a shock absorber). Physiology. Falls (NB axial loading) Sports injuries Fights RTCs


Head Injuries
E N D
Presentation Transcript
1,000,000 Pt’s /yr in A&E • 6000 severe – 40-50% die • Biggest killer for 15-24’s Head Injuries
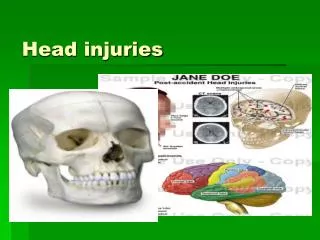
Skin • Skull • Meninges • Brain • Brain sits in CSF fluid (acts as a shock absorber) Physiology
Falls (NB axial loading) • Sports injuries • Fights • RTCs • Get lots of info about M.O.I: • When? • How fast? • How high? • Where hit? • How many impacts? Head Injury causes
Skull fracture • Contusion & laceration • Concussion • Extradural haemotoma • Subdural haemotoma(slow killer – after 3 days – mortality ~50%) • ‘Compression’ (rise in ICP) • Primary & secondary damage What can go wrong?
Shaking of the brain • Temporary disturbance of function (‘stunned’) • Usually no long term damage • Symptoms? Concussion
Headache (mild, generalised) • Dizziness • Nausea • Confusion • Loss of memory • L.O.C • Visual disturbances • Concussion may be related to basilar skull fracture. Concussion: Symptoms
Increased ICP (bleeding or swelling) • May occur straight after injury • …OR days after! • (so always ask about recent head injuries) • Symptoms? Compression
Deteriorating level of response (AVPU) • Intense headache • Nausea / vomiting • Noisy breathing becoming shallow • Slow, strong pulse • One-sided weakness / paralysis • Drowsiness • Change in personality • Severe amnesia • Posturing • Unequal pupils (NB late sign!) • Seizures • Lucid intervals Compression: Symptoms
Increased BP Cushing’s Triad • Decreased Pulse rate • Irregular breathing rate
Requires significant trauma • Bruising usually develops a long time after the event Skull Fracture
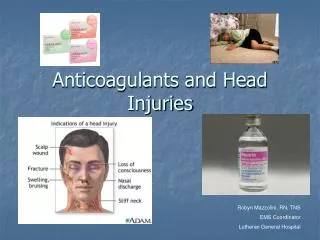
Danger (fights etc) • Scene size-up (M.O.I) • Response (AVPU) • Airway (teeth, blood, L.O.C) • C-Spine!! • Vomiting • Breathing (rate, regularity, depth) • Circulation (pulse, bleeding, skin colour) • Disability / dysfunction • Event history – when depends on seriousness of Pt 999? Assessment: Primary Survey
Feel the scalp – deformity / swelling / bleeding? • Check for CSF fluid(inside!) • Check pupils(NB – alcohol/drugs) • Level of response – A? V? P? U? • Eyes • Speech • Motor response (squeeze fingers both sides) • GCS score (IF you know it well!) • Level of orientation (place, time, event, person) • (But don’t take the piss) Assessment (Dysfunction)
Lots of Obs! • Pulse (rate / regularity / strength) • Breathing (rate / regularity / depth) • If available, ETA / HCP to get BP (or if serious) • Outward signs (e.g. helmet damage) • SAMPLE (inc. alcohol & drugs) • Investigate symptoms & changes • Pins and needles, numbness etc. • If memory loss, what extent? • If L.O.C, how long for? More than once? • Changes in level of orientation (place, time, event, person) • Investigate behaviour More Assessment! NB – Complicated by alcohol
C-spine? (Jaw thrust?) • Position (sat up? Recovpos?) • Oxygen • HCP? Hospital? 999? • Sort wounds (inspect fist!) • CSF fluid? • Reassure (if hyperventilating, control this) • Paracetamol? • Head injury advice (next slide) • Advise not to drink / get high • Advise not to ‘get back on the pitch’ • Advise they’re watched by a friend (why?) Management • And more OBS!
drowsiness • Worsening headache • Confusion & memory loss • Behaviour changes • One-sided weakness • Dizziness • Visual disturbances • Bleeding / CSF • Breathing problems • Vomiting • ..Well.. bad stuff. Namely: Look out for… • NOTE – do they have CAPACITY?? Do they understand what’s going on? Can they remember & repeat the information?
http://www.nhs.uk/Conditions/Head-injury-minor/Pages/Treatment.aspxhttp://www.nhs.uk/Conditions/Head-injury-minor/Pages/Treatment.aspx • http://www2.warwick.ac.uk/fac/med/research/hsri/emergencycare/prehospitalcare/jrcalcstakeholderwebsite/guidelines/head_trauma_2006.pdf Sources