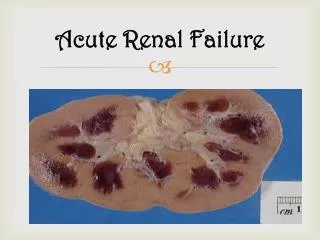
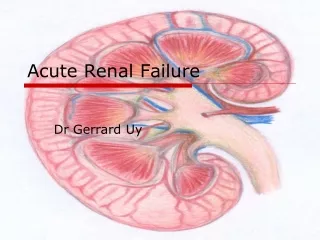
Acute Renal Failure
Acute Renal Failure. A. Symptoms Polyuria, Oliguria or Anuria hematuria Dysuria Uremia Definition: symptomatic azotemia Acidosis (± tachypnea) Mental Status changes Hypervolemia / Hypertension Hyperkalemia Pericarditis. Duration <3 months Oliguria <400 ml urine/24 hours

Acute Renal Failure
E N D
Presentation Transcript
Acute Renal Failure A. Symptoms • Polyuria, Oliguria or Anuria hematuria • Dysuria • Uremia • Definition: symptomatic azotemia • Acidosis (± tachypnea) • Mental Status changes • Hypervolemia / Hypertension • Hyperkalemia • Pericarditis
Duration <3 months • Oliguria <400 ml urine/24 hours • Absolute increase Scr by 0.5 or 1.0 mg/dl or relative increase 25% • Cockcroft – Gault Equation (140-age) x wt(kg) ------------------------ Serum Cr x 72
B. Etiologies • Location of Lesion • Prerenal - ~70% of cases • Intrinsic - ~25% of cases • Post-renal (obstructive) - <5% of cases • FeNa= urine Na x serum Cr ------------------------------- X 100 serum Na x urine Cr Prerenal Renal (ATN) Urine Na <10 >10 FeNa <1% >1% response IVF good poor BUN/Scr >20 nl
Pre-renal azotemia • Decreased effective arterial volume • CHF,,Cirrhosis,,Nephrotic syndrome,,Sepsis • Renal Artery Stenosis (atherosclerosis, fibromuscular dysplasia) • Cardiopulmonary bypass (>3 hours) • Intravascular volume depletion • GI loss…Vomiting..diarrhea…etc • Renal loss diuretc..osmotic diuresis..etc • Cutaneous loss hyperthermia..burns • Hemorrhage • Third space pancreatitis..severe hypoalbuminemia..cappillary leak
II.Parenchymal Damage • Nephritis (inflammation): glomerular vs. interstitial • Tubular Injury: most common cause of ARF Nephrotic Syndrome (total protein losses) III. Obstruction of Outflow (~5%) Urinary Tract Infection (UTI) with Pyelonephritis • Urinary Calculus disease (renal stones) • Crystal Deposition • Bladder tumors with extensive invasion • Prostatic Enlargement: BPH vs. Carcinoma • Unilateral obstruction with only one functioning kidney
Vascular hypertension • Atherosclerotic (atheroembolism) - cholesterol emboli, 5-10% of hospitalized ARF Trauma • Vasculitides • Post-operative - aortic aneurysm repair, aortic cross-clamping • Vasoconstricting Agents - NSAIDs, vasopressors
Drug Induced • ACE Inhibitors • Radiocontrast Dye Interstitial Nephritis - sulfonamides, NSAIDS, other antibiotics • Amphotericin • Cis-Platinum • Aminoglycosides • Non-steroidal anti-inflammatory drugs (NSAIDs)
Pathophysiology • Ischemia is the underlying problem in ARF • leads to depletion of cellular ATP and release of calcium • Reactive oxygen species produced leading to further cell death • Calcium release leads to phospholipase activation • Neutrophils may mediate reperfusion injury (ICAM-1 is involved) • Many nephrotoxins are renal vasocontrictors (eg. cyclosporine, radiocontrast)
C. Initial Evaluation • Consider possible etiologies and direct evaluation • Medications should always be suspected • Standard Blood Testing • Electrolyte/renal panel, Ca2+, Phosphate, Mg2+, Albumin • Complete Blood Count • Foley catheter to rule out bladder obstruction
Urine for electrolytes, dipstick and microscopic analysis • Osmolality, creatinine, Na+, K+, Cl- • Urine spot protein to creatinine ratio (normal is <0.2) • Pigment: Hemoglobin (myoglobin) • Cells, Casts, Crystals, Organisms • Consider Urine culture
Renal/Pelvic Sono - stones, hydronephrosis, mass • Consider Abdominal radiograph if ultrasound is not done to rule out stones • ESR, ASO titer, ANA, C3/C4 Anti-GBM Abs • Renal Biopsy in rapidly progressing disease • ANCA and Anti-GBM diseases - consider cyclophosphamide + glucocorticoids • Idiopathic rapidly progressive glomerulonephritis often ANCA positive (other inflammatory diseases such as bacterial endocarditis can given ANCA+)
Pathology Summary • Glomerular Involvement • Diffuse: all glomeruli in a section are diseased • Focal: some glomeruli in a section are diseased • Segmental: parts of individual glomerulus affected 2.Focal Glomerulonephritis: • Some glomeruli are dead( necrosis, collapse, sclerosis b.Acute or chronic inflamation is often seen 3.Crescent Glomerulonephritis (very poor prognosis) • Crescent (moon shaped) formation in glomerulus • Affected glomeruli are non-functional
Focal and Segmental Glomerulosclerosis: portions of many glomeruli are destroyed 5. Minimal Change Glomerulonephritis a. Glomeruli appear okay, but function is poor b. Electron microscopic evidence of basement membrane disease c. Response to glucocorticoids is usually very good 6. IgA Deposition a.IgA nephropathy b.Deposition of IgA immune complexes c.Differential includes Systemic Lupus (SLE) and Henoch-Schonlein Purpura (HSP)
7. Proliferative Glomerulonephritis a. Increase in mesangeal cell number b. Usually follows insults (eg. Post-Streptococcal) • May be seen in collagen vascular disease, SLE 8. Collapsing Glomerulonephritis • Major form seen in HIV nephropathy • Usually late stage • Rapid progression to renal failure (weeks-months) • No effective therapy to date
9. Tubular Necrosis a. Tubular cells die and slough off basement membrane b. The dead tubular cells form casts which can occlude lumen c. Glomular basement membrane may also be damaged
E. Management • Renal Diet • Low phosphate, potassium, sodium, and protein • High calcium and vitamin D • Various multivitamin formulas available for renal patients, eg. Nephrovit® • Low protein diet may slow progression slightly in chronic renal disease • Phosphate and Calcium • Dangerous if product of Calcium and Phosphage > ~70 (mg/dl) (will lead to precipitation)
If product is close to 70, then phosphate should be lowered with aluminum compounds • These compounds should be given with meals to bind the phosphate directly • If product is <60, then calcium should be given 500-1000mg po tid with meals • If calcium is low but phosphate normal, then calcium should be given before meals • Consider using 1,25 dihyroxyvitamin D supplements
1. Acidosis • Renal tublar acidosis (RTA) is common in early renal failure • Oral bicitra (citrate replaces bicarbonate) may be used • Bicitra is contraindicated in edematous states due to high sodium content 2. Hyperuricemia • Check uric acid levels • Uric acid deposition in renal tubules may worsen progression of renal failure • Allopurinol may be given (100-200mg po qd) to attempt normalization of uric acid
3. Hypertension a. ACE inhibitors generally contraindicated in moderate to severe renal failure • Calcium blockers such as nifedipine • Labetolol is also very effective but patient should have LV EF>50% and no bronchospasm d. Consider Hydralazine for afterload reduction e. Pure alpha-adrenergic blocking agents may be effective, but tachyphylaxis may occur • Diuretic improve hypertension/ volume overload
4. Volume overload a. Attempt to maximize cardiac output and improve intravascular volume b. Diuretics often worsen renal failure but may be necessary to prevent pulmonary edema c. In general, potassium sparing diuretics should be avoided (high risk hyperkalemia) e. Dopamine or mannitol can be tried, but are usually not effective f. Albumin infusions are probably not helpful, but may help diuresis in low albumin states g. Dialysis may be required particularly in severe volume overload situations
5. Protein Load • Reducing protein load is thought to reduce azotemia • Appears to slow progression of CRF • Patients with moderate renal disease - some decrease in progression on low protein diet • Patients with severe renal disease show no benefit on low protein diet 6. Hospital inpatients with ARF ~50% mortality rate
7. Newer Agents • Atrial natriuretic factor (ANF)= dilators + diuretic • ANF (Auriculin®) ? efficacy in oliguric ARF • ANF may increase renal dysfunction in diabetics receiving radiocontrast • Brain derived natriuretic factor (BDNF) may be effective some patients • Other vasodilators (eg. calcium channel blockers) are not effective • Investigation renal growth/regeneration factors
8. Dialysis Indications • Serum abnormalities unresponsive to medical therapy • Severe Acidosis • Severe Hyperkalemia II Uremia • Mental status changes (usually delirium) • Nausea and vomiting • Pericarditis (pericardial friction rub)
III Volume Overload • Hemofiltration or hemodialysis can be used to allow recovery of kidney after ARF • Average duration of need for these therapies was 9 days in ARF • After this time, kidneys regain function and increase urine output • Native kidneys may continue with minimal function for 6-12 months of hemodialysis • After that, native kidneys usually shut down permanently
Kidney Transplantation • Excellent (and improving) results with cadaveric grafts. • Living Related Donor kidneys superior to CRT • New kidney usually placed in extraperitoneally in the pelvis • Cyclosporin ,Prednisone, OKT3, mycophenolic acid, FK506 immunosuppression • Combined Kidney Pancreas transplant in Diabetic ESRD patients