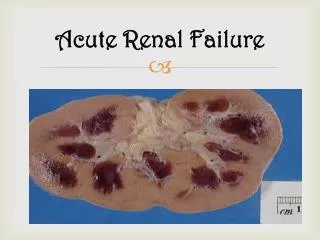
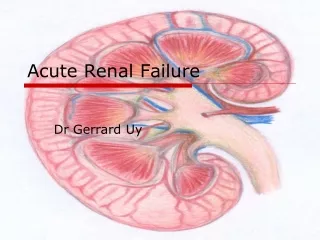
Acute Renal Failure
Acute Renal Failure. Dr. Belal Hijji, RN, PhD April 9 & 16, 2012. Learning Outcomes. At the end of this lecture, students will be able to: Define renal failure and discuss its pathophysiological changes. Describe the categories of acute renal failure (ARF).

Acute Renal Failure
E N D
Presentation Transcript
Acute Renal Failure Dr. Belal Hijji, RN, PhD April 9 & 16, 2012
Learning Outcomes At the end of this lecture, students will be able to: • Define renal failure and discuss its pathophysiological changes. • Describe the categories of acute renal failure (ARF). • Recognise the clinical manifestations of ARF. • Discuss the assessment and diagnostic findings associated with ARF. • Describe the medical management of a patient with ARF. • Discuss the nursing interventions designed to meet specific goals associated with ARF.
Renal Failure • Renal failure results when the kidneys cannot remove the body’s metabolic wastes (urea) or perform their regulatory functions. The wastes accumulate in the body fluids, leading to a disruption in endocrine and metabolic functions as well as fluid, electrolyte, and acid–base disturbances. Renal failure is a systemic disease and is a final common pathway of many different kidney and urinary tract diseases.
Acute Renal Failure • Pathophysiology: Acute renal failure (ARF) is a sudden and almost complete loss of kidney function over a period of hours to days. ARF manifests with oliguria (less than 400 mL/day of urine), anuria (less than 50 mL/day of urine), or normal urine volume. The patient has high serum creatinine and BUN levels (azotemia) and retention of other metabolic waste products normally excreted by the kidneys.
Categories of Renal Failure • Prerenal conditions occur as a result of impaired blood flow that leads to hypoperfusion of the kidney and a drop in the GFR. The causes could be hemorrhage, myocardial infarction, heart failure, or cardiogenic shock, sepsis or anaphylaxis. • Intrarenal causes of ARF are the result of actual parenchymal damage to the glomeruli. Conditions such as burns, crush injuries, and infections, nephrotoxic agents (nonsteroidal anti-inflammatory drugs (NSAIDs); angiotensin-converting enzyme (ACE) inhibitors), may lead to acute tubular necrosisand cessation of renal function. With burns and crush injuries, myoglobin (a protein released from muscle when injury occurs) and hemoglobin are liberated, causing renal toxicity, ischemia, or both.
Categories of Renal Failure (Continued…) • Postrenal causes of ARF are usually the result of an obstruction somewhere distal to the kidney. Pressure rises in the kidney tubules; eventually, the GFR decreases. Common causes include calculi (stones), tumors, benign prostatic hyperplasia, strictures, and blood clots.
Clinical Manifestations • Almost every system of the body is affected when there is failure of the normal renal regulatory mechanisms. • The patient may appear critically ill and lethargic [يميل للنوم], with persistent nausea, vomiting and diarrhea. The skin and mucous membranes are dry from dehydration, and the breath may have the odor of urine. Central nervous system signs and symptoms include drowsiness, headache, muscle twitching [ارتعاش], and seizures [نوبات مرضية]. Next slide summarizes some common clinical findings for all three categories of ARF.
Assessment and Diagnostic Findings • Changes in urine: Please refer to the previous slide to see the urine changes based on the type of ARF. • Increased BUN and creatinine levels: Rise in the BUN depends on the degree of catabolism (breakdown of protein), renal perfusion, and protein intake. Serum creatinine levels are useful in monitoring kidney function and disease progression. • Hyperkalemia: With a declining GFR, the patient cannot excrete potassium normally. Protein catabolism results in the release of cellular potassium into the body fluids, causing severe hyperkalemia. Hyperkalemia may lead to dysrhythmias and cardiac arrest.
Medical Management • The kidney has a remarkable ability to recover from insult. The objectives of treatment of ARF are to restore normal chemical balance and prevent complications. • The medical management includes maintaining fluid balance, avoiding fluid excesses, or possibly performing dialysis. • Maintenance of fluid balance is based on daily body weight, serial measurements of central venous pressure, serum and urine concentrations, fluid losses, blood pressure, and the clinical status of the patient. The parenteral and oral intake and the output, including insensible loss, are calculated and are used as the basis for fluid replacement.
Medical Management (Continued…) • Because excessive administration of parenteral fluids may cause pulmonary edema, extreme caution must be used to prevent fluid overload (Characterised by dyspnea, tachycardia, distended neck veins, and crackles) . Generalized edema is assessed by examining the presacral and pretibial areas several times daily. Mannitol, furosemide, or ethacrynic acid may be prescribed to initiate a diuresis and prevent or minimise subsequent renal failure. • Adequate blood flow to the kidneys in patients with prerenal causes of ARF may be restored by intravenous fluids or blood product transfusions. • Dialysis may be initiated to prevent serious complications of ARF, such as hyperkalemia, severe metabolic acidosis, pericarditis, and pulmonary edema.
Pharmacologic Therapy[Hyperkalemia] • Hyperkalemia is a life-threatening condition. Therefore, the patient is monitored for: • Serum potassium levels • Electrocardiogram (ECG) changes (tall, tented, or peaked T waves) (next slide) • Signs and symptoms (muscle weakness, diarrhea, abdominal cramps) Schematic representation of normal ECG
Pharmacologic Therapy (Continued…) • Hyperkalemia may be reduced by administering cation-exchange resins (sodium polystyrene sulfonate [Kayexalate]) orally or by retention enema. Kayexalate exchanges a sodium ion for a potassium ion in the colon (major site for potassuim exchange). Sorbitol is often administered in combination with Kayexalate to induce a diarrhea-type effect. • Administration of a retention enema requires a rectal catheter with a balloon to facilitate retention for 30 to 45 minutes. Afterward, a cleansing enema is administered to remove the Kayexalate resin as a precaution against fecal impaction. • Immediate dialysis. • Intravenous glucose and insulin or calcium gluconate may be used as emergency measures to treat hyperkalemia.
Nursing Management of ARF • Monitoring fluid and electrolyte balance. The nurse: • monitors the patient’s serum electrolyte levels and physical indicators of fluid and electrolyte imbalances. • carefully screens parenteral fluids, all oral intake, and all medications to ensure that hidden sources of potassium are not inadvertently administered or consumed. • monitors the patient closely for signs and symptoms of hyperkalemia (Slide 12). • monitors fluid status by paying careful attention to fluid intake, urine output, apparent edema, distention of the jugular veins, breath sounds, and increasing difficulty in breathing. • maintains accurate daily weight, and intake and output record. • reports to physician indicators of deteriorating fluid and electrolyte status, and prepares for emergency treatment.
Nursing Management of ARF (Continued…) • Reducing metabolic rate. The nurse: • shouldreduce the patient’s metabolic rate to reduce catabolism and the subsequent release of potassium and accumulation of waste products (urea and creatinine). • may keep the patient on bed rest to reduce exertion and the metabolic rate during the most acute stage of ARF. • should prevent or promptly treat fever and infection to decrease the metabolic rate and catabolism.
Nursing Management of ARF (Continued…) • Promoting pulmonary function. The nurse: • assist the patient to turn, cough, and take deep breaths frequently to prevent atelectasis and respiratory tract infection. • Preventing infection. The nurse: • strictly observes aseptic technique when caring for the patient to minimise the risk of infection and increased metabolism. • avoids, when possible, inserting an indwelling urinary catheter as it is a high risk for urinary tract infection (UTI).