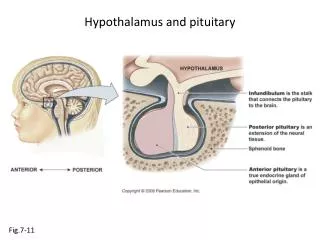
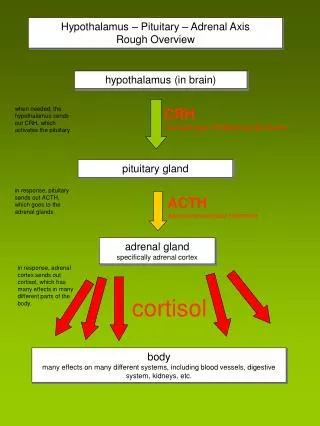
Hypothalamus and Pituitary
370 likes | 957 Vues
Hypothalamus and Pituitary. Endocrine Control: Three Levels of Integration. Hypothalamic stimulation–from CNS Pituitary stimulation–from hypothalamic trophic Hs Endocrine gland stimulation–from pituitary trophic Hs. HYPOTHALAMUS AND ANTERIOR PITUITARY LOBE.

Hypothalamus and Pituitary
E N D
Presentation Transcript
Endocrine Control: Three Levels of Integration • Hypothalamic stimulation–from CNS • Pituitary stimulation–from hypothalamic trophic Hs • Endocrine gland stimulation–from pituitary trophic Hs
HYPOTHALAMUS AND ANTERIORPITUITARY LOBE • The hypothalamic hormones either promote or inhibit release of the anterior pituitary hormones
Endocrine Control: Three Levels of Integration Figure 7-13: Hormones of the hypothalamic-anterior pituitary pathway
Characteristics of hypothalamic releasing hormones • Secretion in pulses • Act on specific membrane receptors • Transduce signals via second messengers • Stimulate release of stored pituitary hormones • Stimulate synthesis of pituitary hormones • Stimulates hyperplasia and hypertophy of target cells
HORMONES AND THE HYPOTHALAMUS The hypothalamus is the major regulatory area for the internal environment, acting as an interface between the two control systems, the nervous system and the endocrine system. As well as controlling the activities of the autonomic nervous system. It produces a large number of Releasing hormones involved directly or indirectly in: • maintenance of homeostasis • management of stress, i.e. disturbance of Homeostasis • determination of the size, shape and sexual characteristics of the body – morphogenesis.
NEURAL CONNECTIONS • The hypothalamus receives information from many parts of the nervous system. These include receptor cells which monitor many aspects of the body’s internal environment: • pressures in the circulation • osmotic pressure and the state of the body’s fluid balance • composition of the body fluids, e.g. pH, electrolytes, • glucose • body temperature • regulation of food intake.
Hypothalamic releasing hormone Effect on pituitary Corticotropin releasing hormone (CRH) Stimulates ACTH secretion Thyrotropin releasing hormone (TRH) Stimulates TSH and Prolactin secretion Growth hormone releasing hormone (GHRH) Stimulates GH secretion Somatostatin Inhibits GH (and other hormone) secretion Gonadotropin releasing hormone (GnRH) a.k.a LHRH Stimulates LH and FSH secretion Prolactin releasing hormone (PRH) Stimulates PRL secretion Prolactin inhibiting hormone (dopamine) Inhibits PRL secretion Hypothalamic releasing hormones
Anterior pituitary • Anterior pituitary: connected to the hypothalamus by hypothalmoanterior pituitary portal vessels. • The anterior pituitary produces six peptide hormones: • prolactin, • growth hormone (GH), • thyroid stimulating hormone (TSH), • adrenocorticotropic hormone (ACTH), • follicle-stimulating hormone (FSH), • luteinizing hormone (LH).
ANTERIOR PITUITARY SECRETES TROPIC HORMONES IN PULSATILE FASHION
ANTERIOR PITUITARY HORMONES Growth Hormone (GH, Somatotropin): primary hormone responsible for regulating body growth, and is important in metabolism Thyroid-stimulating Hormone (TSH): stimulates secretion of thyroid hormone & growth of thyroid gland Adrenocorticotropic Hormone (ACTH): stimulates cortisol secretion by the adrenal cortex & promotes growth of adrenal cortex
ANTERIOR PITUITARY Follicle-stimulating Hormone (FSH):Females: stimulates growth & development of ovarian follicles, promotes secretion of estrogen by ovaries. Males: required for sperm production Luteinizing Hormone (LH):Females: responsible for ovulation, formation of corpus luteum in the ovary, and regulation of ovarian secretion of female sex hormones. Males: stimulates cell in the testes to secrete testosterone Prolactin:Females: stimulates breast development and milk production. Males: involved in testicular function
POSTERIOR PITUITARY Hormones synthesized in the hypothalamus are transported down the axons to the endings in the posterior pituitary Hormones are stored in vesicles in the posterior pituitary until release into the circulation Principal Hormones: Vasopressin & Oxytocin
Figure 7-12: Synthesis, storage, and release of posterior pituitary hormones
POSTERIOR PITUITARY Oxytocin: Synthesized as the precursor hormone: prepro-oxyphysin Action primarily on the breasts and uterus
POSTERIOR PITUITARY Vasopressin or Antidiuritic Hormone Plasma osmolality is monitored by osmoreceptors in the hypothalamus Increases in plasma osmolality stimulates secretion of vasopressin Small changes above normal plasma osmotic pressure ( 285 mosm/kg) stimulate release of vasopressin
Physiologic Effects of Antidiuretic Hormone • Effects on the Kidney • The single most important effect of Antidiuretic hormone is to conserve body water by reducing the output of urine. • Injection of small amounts of Antidiuretic hormone into a person or animal results in Antidiuresis or decreased formation of urine, and the hormone was named for this effect. • A diuretic is an agent that increases the rate of urine formation.
Antidiuretic hormone binds to receptors in the distal or collecting tubules of the kidney and promotes reabsorbtion of water back into the circulation. • In the absence of Antidiuretic hormone, the kidney tubules are virtually impermeable to water, and it flows out as urine.
Control of Antidiuretic Hormone Secretion • The most important variable regulating Antidiuretic hormone secretion is plasma osmolarity, or the concentration of solutes in blood. • Osmolarity is sensed in the hypothalamus by neurons known as an osmoreceptors, and those neurons, in turn, simulate secretion from the neurons that produce Antidiuretic hormone. • When plasma osmolarity is below a certain threshold, the osmoreceptors are not activated and Antidiuretic hormone secretion is suppressed
Secretion of antidiuretic hormone is also simulated by decreases in blood pressure and volume, conditions sensed by stretch receptors in the heart and large arteries. • Changes in blood pressure and volume are not nearly as sensitive a stimulator as increased osmolarity, but are nonetheless potent in severe conditions. • For example, Loss of 15 or 20% of blood volume by hemorrhage results in massive secretion of Antidiuretic hormone.
Disease States • The most common disease of man and animals related to Antidiuretic hormone is diabetes insipidus • Hypothalamic ("central") diabetes insipidus results from a deficiency in secretion of antidiuretic hormone from the posterior pituitary. • Nephrogenic diabetes insipidus occurs when the kidney is unable to respond to antidiuretic hormone.
The major sign of either type of diabetes insipidus is excessive urine production.
PATHOPHYSIOLOGICAL CHANGES IN ADH SECRETION Effects of Primary Polydipsia, Diabetes Insipidus and SIADH