Neck Trauma
Neck Trauma. Rivera, Rivere , Robosa , Rodas , Rodriguez, Rogelio, Roque , Ruanto. stab wound at the right side of the neck at the level of the cricoid. Background. Few emergencies pose as great a challenge as neck trauma.


Neck Trauma
E N D
Presentation Transcript
Neck Trauma Rivera, Rivere, Robosa, Rodas, Rodriguez, Rogelio, Roque, Ruanto
stab wound at the right sideof the neck at the level of thecricoid
Background • Few emergencies pose as great a challenge as neck trauma. • Because a multitude of organ systems (eg, airway, vascular, neurological, gastrointestinal) are compressed into a compact conduit, a single penetrating wound is capable of considerable harm
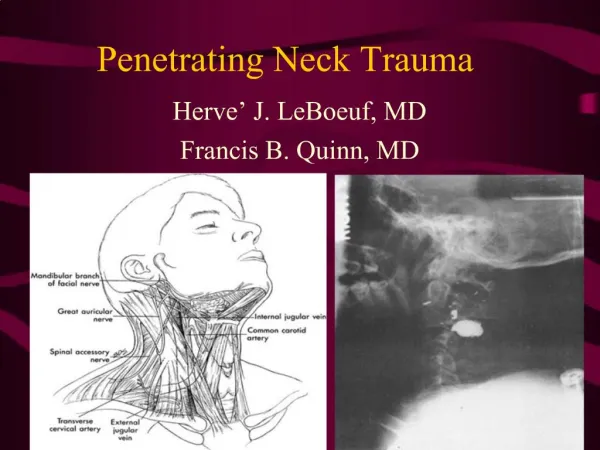
Anatomic zones • Dividing the neck into anatomic zones or regions assists in the evaluation of injury. • The sternocleidomastoid separates the neck into anterior and posterior triangles. • Most of the important vascular and visceral organs lie within the anterior triangle bounded by the sternocleidomastoid posteriorly, the midline anteriorly, and the mandible superiorly.
Zone I the base of the neck, is demarcated by the thoracic inlet inferiorly and the cricoid cartilage superiorly. Zone II encompasses the midportion of the neck and the region from the cricoid cartilage to the angle of the mandible. Zone III characterizes the superior aspect of the neck and is bounded by the angle of the mandible and the base of the skull. Anatomic Zones
Zone I great vessels (subclavian vessels, brachiocephalic veins, common carotid arteries, aortic arch, and jugular veins, trachea, esophagus, lung apices, cervical spine, spinal cord, and cervical nerve roots Zone II carotid and vertebral arteries, jugular veins, pharynx, larynx, trachea, esophagus, and cervical spine and spinal cord Zone III salivary and parotid glands, esophagus, trachea, vertebral bodies, carotid arteries, jugular veins, and major nerves (including cranial nerves IX-XII) Structures at risk
Penetrating Trauma • Vascular injuries arising from penetrating trauma may occur directly, causing a partial or complete transection of the vessel or inducing formation of an intimal flap, arteriovenous fistula, or pseudoaneurysm. • Thrombosis • 25-40% • Common sites: • internal jugular vein (9%) • carotid artery (7%) • pharynx or the esophagus occurs in 5-15% • larynx or the trachea 4-12% • Major nerve injury occurs in 3-8% of patients sustaining penetrating neck trauma. Spinal cord injury occurs infrequently and almost always results from direct injury rather than secondary osseous instability.
Blunt Trauma • motor vehicle crashes • sports-related injuries • clothesline tackle • strangulation • blows from the fists or feet • excessive manipulation (ie, any manual operation such as chiropractic treatment or physical realignment or repositioning of the spine).
Direct forces can shear the vasculature. • Excessive rotation and/or hyperextension of the cervical spine causes distention and stretching of the arteries and veins producing shearing damage and resultant thrombosis. • Intraoral trauma may extend to the cerebral blood supply. Basilar skull fractures may disrupt the intrapetrous portion of the carotid artery. • Impact to the exposed anterior aspect of the neck may crush the larynx or the trachea, particularly at the cricoid ring, and compress the esophagus against the posterior spinal column. • A sudden increase in intratracheal pressure against a closed glottis (eg, improper wearing of a seat belt), a crush bruise (eg, clothesline tackle), or a rapid acceleration-deceleration action may cause a tracheal injury.
Neck Injury – Zones I, II, III Zone I – angle of mandible to base of skull Zone II – cricoid cartilage to angle of mandible Zone III (thoracic inlet) - sternal notch to cricoid cartilage Townsend: Sabiston Textbook of Surgery, 18th ed.
Airway • Early orotracheal intubation • Oxygenation
Breathing • Check for concomitant injuries or presence of pneumothorax
Circulation • Digital control of the bleeding • IV access and judicious fluid resuscitation • 1L IV bolus of normal saline, Ringer’s lactate or other isotonic crystalloid solution • Packed red blood cell
Disability • Check for neurologic signs
Exposure • Check for other wounds
Operation • Prompt wound exploration
Clinical Indications for Neck Exploration Vascular Expanding hematoma External hemorrhage Diminished carotid pulse Airway Stridor Hoarseness Dysphonia / voice change Hemoptysis Subcutaneous air Digestive Tract Dysphagia / odynophagia Subcutaneous air Blood in oropharynx Neurologic Lateralized neurologic deficit consistent with injury Altered state of consciousness not caused by head injury conscious, coherent, agitated; talks in phrases; VS: BP = 90/60 PR = 100/min RR = 25/min Townsend: Sabiston Textbook of Surgery, 18th ed.
Penetrating injury in Zone II for Neck Exploration • Preoperative workup in this subset of patients is minimal. • Patients with penetrating injuries in zone II are generally taken directly to surgery • Patients with injuries in zone I and zone III should undergo preoperative radiographic vascular imaging, if possible. Townsend: Sabiston Textbook of Surgery, 18th ed.
Penetrating Injury in Zone II, stable asymptomatic • Optimal approach controversial: • Mandatory surgical exploration for all penetrating injuries because of a low rate of complications and the potentially devastating effect of delay in the diagnosis of aerodigestive tract injuries. • Selective exploration based either on the results of extensive evaluation, including angiography, esophagoscopy, and esophagography, or on progression of clinical symptoms. • Work-ups are usually done on patients with: • Neck injury in zone II, stable and asymptomatic • Neck injury in zones I and III • Blunt neck trauma • Work-ups: CT scan is advocated Townsend: Sabiston Textbook of Surgery, 18th ed.
Surgical Neck Exploration • Neck exploration should be performed in the operating room under general endotracheal anesthesia • Hemodynamically stable patient with a patent airway – intubation can be deferred until laryngoscopy and bronchoscopy have been performed • Nasogastric tube is passed to ensure an empty stomach • Chest auscultation
Management of Specific Injuries • Blood vessels – most commonly injured • Hemostasis should be maintained by direct pressure or digital occlusion until proximal and distal control of vessel is achieved • Choice of graft material should be based on size • Polytetrafluorethylene is commonly used
Management of Specific Injuries: Airway Injuries Signs of larynx or trachea injury: • Voice alteration • Hemoptysis • Stridor • Drooling • Sucking, hissing, or air frothing or bubbling through the neck • Subcutaneous emphysema and/or crepitus • Hoarseness • Dyspnea • Distortion of the normal anatomic appearance (eg, loss of normal landmarks, asymmetry, flattened thyroid prominence, tracheal deviation) • Pain on palpation or with coughing or swallowing • Pain with tongue movement implies injury to the epiglottis, hyoid bone, or laryngeal cartilage • Crepitus (This hallmark sign of disruption to aerodigestive tract is noteworthy in only one third of cases.) http://emedicine.medscape.com/article/827223-overview
Airway Injuries Penetrating injuries to the airway • either clinically overt, with bubbling and air movement through the wound, or found at the time of neck exploration performed for other indications. • Blunt laryngotracheal injuries • the diagnosis is generally established through a combination of neck CT, direct laryngoscopy, and bronchoscopy. • The need for operative intervention for laryngeal trauma is determined by the degree of anatomic derangement and mucosal integrity in the larynx. Male with tracheal laceration from masonery saw. ETT inserted through wound. Nil great vessel damage. Required tracheostomy.
Airway Injuries • Lacerations are débrided and closed primarily Simple lacerations of the trachea • repaired by direct suture • If there is significant tissue loss, the trachea can usually be mobilized sufficiently to allow for the loss of about two tracheal rings without undue difficulty. Loss of a larger portion of trachea may necessitate tracheostomy or complex reconstructive procedures. Laryngeal injuries • treated by closure of mucosal lacerations and reduction of cartilaginous fractures • careful anatomic reconstruction, if possible, is critical • difficult to treat
Management of Specific Injuries: Pharynx and Esophagus • If the diagnosis is made early • primary surgical repair is generally possible. • If the diagnosis is delayed for > 12 hours • primary repair may be impractical diversion and drainage being the only alternative • The major morbidity and mortality associated with esophageal injuries are the result of delay in diagnosis
Pharynx and Esophagus Signs of esophagus and pharynx injury • Dysphagia • Bloody saliva • Sucking neck wound • Bloody nasogastric aspirate • Pain and tenderness in the neck • Resistance of neck with passive motion testing • Crepitus • Bleeding from the mouth or nasogastric tube http://emedicine.medscape.com/article/827223-overview
The basic approach to esophageal injuries: • The esophagus must be sufficiently mobilized to allow full evaluation of the wound and careful débridement of devitalized tissue. • The injury should be repaired primarily if possible, either by a one-layer or two-layer technique. • If the tissue loss is sufficient to preclude primary repair, cervical esophagostomy should be performed as a temporizing measure, with plans for complex reconstruction of the esophagus after the initial trauma has resolved. • A drain should be left in place after all esophageal repairs.
Diagnostic Procedures Radiography • Upper and mid esophageal perforations The most frequent site of these perforations is at the level of the cricopharyngeus muscle, and most perforations are iatrogenic. The conventional radiographic findings include widening of the precervical soft tissues, air in the precervical soft tissues, widening of the superior mediastinum, and a right-sided hydrothorax. http://emedicine.medscape.com/article/375584-imaging
Water-soluble contrast study of the upper esophagus shows leakage of contrast material after instrumentation. Cervical abscess following esophageal injury subsequent to endotracheal intubation. Note the increased soft tissue prevertebral space and air in the soft tissues http://emedicine.medscape.com/article/375584-imaging
Diagnostic Procedures Computed Tomography • CT findings in esophageal tear/perforation: • Extraluminal air in the mediastinum or surrounding the esophagus is the most reliable sign and, when taken in conjunction with the clinical presentation, has a 92% accuracy. Gas may appear as a single or multiple discrete collections, particularly with mediastinal abscess formation. Air fluid levels may also be seen within mediastinal abscesses. • Other findings include obliteration of fat planes in the mediastinum resulting from inflammation, periesophageal/mediastinal fluid, esophageal thickening, pleural effusions (usually unilateral), extravasation of oral contrast material into the periesophageal tissues, and a tract at the site of the tear http://emedicine.medscape.com/article/375584-imaging
Nonenhanced CT scan through the mid esophagus in a patient with esophageal perforation after upper GI endoscopy shows a false tract emanating from the esophagus (arrow). Nonenhanced CT scan through the mid esophagus in a patient with esophageal perforation after upper GI endoscopy shows leakage of oral contrast material (blue arrow) and air in the posterior mediastinum (red arrow). http://emedicine.medscape.com/article/375584-imaging
Diagnostic Procedures Ultrasonography • Ultrasonography has not been used in the diagnosis of esophageal tears and perforations; however, transesophageal endosonography has been used to evaluate posterior mediastinitis, which is a known complication of esophageal tears http://emedicine.medscape.com/article/375584-imaging
Objective • To assess the impact of the increasing use of MDCT angiography in the setting of blunt and penetrating neck trauma on the use of digital subtraction angiography (DSA)
Background of the Study • Although digital subtraction angiography (DSA) is still accepted as the gold standard for imaging the major vessels of the neck, the reported high number of patients with negative results and the risk associated with performing such procedures have prompted a search for other less invasive imaging techniques. • Noninvasive techniques that have been explored as a potential replacement for catheter angiography in this patient population include MR angiography, duplex sonography, and CT angiography.
Background of the Study • In recent years, CT angiography has also been reported to be useful in the detection of injuries to the major arteries. • Prior studies using single-detector helical CT have shown high sensitivity and specificity for detecting injuries to major vessels of the neck in the setting of both blunt and penetrating trauma.
Patient Population • In general, the patient is considered to be at risk for having an arterial injury and a candidate for diagnostic angiography if one or more of the following signs or symptoms are present: • active bleeding from an unknown source • stable or expanding neck hematoma • neck pain with focal neurologic deficit • palpable bruit or thrill
Methodology • Retrospective: 36 months (Jan 2001 – Dec 2003) • January 2001 to December 2003, 57 patients were referred for CT angiography or DSA of the neck after blunt or penetrating neck trauma • All CT angiograms were acquired with a 4-MDCT scanner • The patients were divided into three groups on the basis of consecutive 12-month periods (2001, 2002, and 2003), and the initial imaging technique was recorded • The results of CT and digital subtraction angiograms were compared with operative findings and with clinical course, when available.
Methodology • Of the 57 patients, 17 underwent both MDCT angiography and DSA during the study period. • The mean age of the study population was 31 years with an age range of 14–90 years. • The mechanism of injury in the study population included gunshot wound (n=21), stab wound (n=12), motor vehicle crash (n=12), assault with a blunt object (n=4), attempted hanging (n=2), fall (n=3), crush injury (n=1), and twisting injury (n=2).
Methodology • CT angiography examinations were reported as positive when one or more of the following findings were present: • arterial dissection, arterial pseudoaneurysm, arterial transection, or arterial occlusion. • Findings were reported as indeterminate if isolated IV contrast extravasation was present without an identifiable arterial injury on the CT images
Results • In 2001, 12 patients were referred for imaging: nine patients were evaluated initially with DSA and three patients were evaluated with CT angiography and subsequently with DSA for further evaluation. • In two of these three patients, CT angiograms showed no abnormality and this result was confirmed with catheter angiography • The third patient underwent DSA for suspected pseudoaneurysm of the superior thyroidal branch of the external carotid artery based on findings present on the initial CT angiography; DSA confirmed this finding
Results • In 2002 and 2003, 11 and 34 patients, respectively, underwent CT angiography as the initial imaging examination. During these 2 years, no patient underwent DSA as the initial diagnostic test, but five patients underwent DSA after CT angiography for the following indications: • evaluation of nondiagnostic CT angiograms (n=1) • confirmation of findings when requested by the clinical service (n=2) • and catheter-guided therapy (n=2)
Results • 2002 • Of the 11 CT angiography examinations, one patient with a gunshot wound to the neck was found to have an occlusion of the left internal carotid artery and dissection of the left vertebral artery • Another patient with a large laceration from a stab wound had negative findings on the initial CT angiogram. This patient was taken to the operating room for wound exploration before repair of the laceration, and a facial vein laceration was repaired • Nine other patients with negative CT angiography findings were managed conservatively, without further intervention or diagnostic imaging