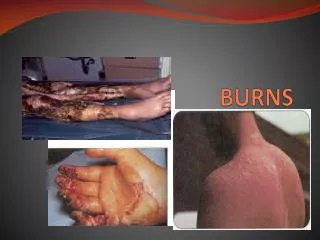
Burns
Burns. Linda Copenhaver. Introduction. Incidence of Burns 450K in U.S. seek medical care annually Approximately 45K are hospitalized Which setting do most burn trauma injuries occur? How many Burn Trauma centers in U.S.?. Types of Burn Injury. Thermal Chemical

Burns
E N D
Presentation Transcript
Burns Linda Copenhaver
Introduction • Incidence of Burns • 450K in U.S. seek medical care annually • Approximately 45K are hospitalized • Which setting do most burn trauma injuries occur? • How many Burn Trauma centers in U.S.?
Types of Burn Injury • Thermal • Chemical • Electrical-what type considered here? Which state has highest incidence of ____ injuries? • Radiation
Thermal Burns( Most Common) • Caused by flame, flash, scald, or contact burns • STOP & DROP • Roll to shut off O2 supply to fire • Flush or immerse in cold water • DO NOT use ICE on deep burns, just localized, superficial burns
Chemical Burns • Remove person from contact with agent • Flush with water continuously • Remove affected clothing if possible • Alkaline agents worse than acid, process keeps going
Electrical burns • Coagulation necrosis • Severity depends on voltage, amount of resistance, time, and current pathways.
Electrical Burn–Back Fig. 25-2 B
Frequently only entry (yellow-white) and exit (blow out) wounds are visible • Current practice: Now refer to contact points vs entry and exit points. • Extensive tissue damage is masked • How can we evaluate “masked tissue damage”???
Electrical Burns (cont) • Patient at risk for arrhythmias due to _____, metabolic acidosis due to _____, and acute tubular necrosis due to ______. • Current can be so strong to fracture long bones and cause respiratory muscles to contract
Cross Section of Skin Fig. 25-3
Depth of Burns Superficial Partial Thickness Burn (1st degree) Epidermis involved Sunburn, UV light, mild radiation, Pink to red Slight edema Mild pain
Depth of Burns • Deep Partial Thickness (2nd) • Epidermis and some of dermis, is painful, red, blisters
Depth of Burns • Deep Partial Thickness (2nd) • Epidermis and Dermis • Very Painful, edema, pale • Moist or dry, but more commonly wet • Blisters
Depth of Burns (cont) • Full Thickness Burns (3rd) • Epidermis, Dermis, and Subcutaneous tissue burned • Nerve endings destroyed • Little or no pain
Depth of Burns (cont) • Full thickness (4th degree) • Involves past the 3 layers down to the bone and/or organs
Rule of Nines Chart; quick & easy Fig. 25-4 B
Lund-Browder Chart; More accurate Fig. 25-4 A
Burn Unit Referral Criteria • Deep Partial Thickness burns > 10% TBSA • Burns that involve the face, hands, feet, genitalia, perineum, or major joints • Full thickness burns in any age group • Electrical burns, including lighting • Inhalation burns requiring intubation • Chemical burns that involve deep and extensive TBSA burned
Medical/Nursing Management of Burns • I. Emergent Phase • Period of time from onset of burns to the beginning of fluid remobilization • Usually lasts 24-48 hours
Emergent Phase (cont) • Also called FLUID ACCUMULATION PHASE • The greatest initial threat to a major burn victim is hypovolemic shock • Let’s do the Patho on p. 479 Lewis…this is a DING DING!
What are the Priorities in this patient??? • Is this patient a candidate for a major burn center?
Nursing Care During Emergent Phase • Impaired Gas Exchange r/t tissue hypoxia secondary to carbon monoxide poisoning • Note: CO poisoning is the MOST immediate cause of death from fire.
Signs & Symptoms of Carbon Monoxide Poisoning • Edema of Airway • Hoarseness • Dysphagia • Stridor • Copius Secretions usually black tinged • Skin will appear cherry red
Interventions for CO Poisoning: • Assess for S&S CO poisoning (mild to severe) • Humidified O2 100% via face mask • High Fowler’s Position • TCDB q 1 hour • Intubation & Ventilation • Bronchodilators for bronchospasm • One other thing…..does anyone know???
Nursing Care during Emergent Phase (cont) • Impaired Gas Exchange r/t mucosal edema throughout respiratory tract secondary to smoke inhalation, hot air, chemical gases
Interventions: • Early intubation to prevent trach placement • Ventilation • Humidified O2 100% • ABG’s • Bronchodilators
Questions to Ask Burn Victims • Were you in an enclosed space? • Were you standing up? • Was it a flame and chemical fire? • Are you having difficulty breathing?
What are your #1 priorities in this patient? Patient #1 Patient #2
Emergent Phase (cont) • Ineffective Breathing pattern r/t constriction of chest/trachea secondary to the effects of full thickness burns. • Assess for signs of constriction • Escharotomies with circumferential burns of chest
Escharotomy of chest and arm • What is the pathophysiology here?
Emergent Phase (cont) • Fluid Volume Deficit (intravascular) r/t massive fluid shift to interstitial spaces • Assess fluid needs: • Brooke Formula • Evans Formula
Parkland Baxter Formula • Most widely used • Formula • LR 4ml X kg body weight X TBSA % burned • ½ total amount given 1st 8 hours • ¼ total amount given next 8 hours • ¼ total amount given next 8 hours
Okay Nurses Let’s Calculate • What would the fluid replacement be for a patient who weighed 60kg and had 30% TBSA burned??? • 1st 8 hours= _____ or ____ml/hr • 2nd 8 hours= _____ or _____ml/hr • 3rd 8 hours= ______ or _____ml/hr
Crystalloids used such as LR, 0.9NS, D5NS • Colloids (albumin, dextran, FFP) used to expand plasma. • Colloids not given until after capillary permeability decreases and returns to normal…..WHY?
Insert foley catheter to monitor output. What should urine output be in an adult??? • Frequent vital signs • SBP>100 • Pulse<100 • RR 16-20
Emergent Phase (cont) • Monitor Electrolytes and Hematocrit; tells you about fluid shift. • What should Hct be doing as time progresses???
Emergent Phase (cont) • Potential for Infection r/t loss of skin and micro invasion • Meticulous hand washing • Sterile technique during dressing changes & wound care • Hair near burned areas shaved
Potential for Infection r/t loss of skin and micro invasion (cont) • Blisters popped or not??? • Tetanus Toxoid I.M. given to all major burn victims to fight anaerobic contamination of burn wound
Hydrotherapy in cart (water is heated to approximately 104 degrees) • < 30 minutes to prevent _____
Hydrotherapy Cart • What does hydrotherapy accomplish?
Wound Care • Open Method • Apply topical chemotherapy
Topical Meds/Antimicrobials • Silvadene cream • Silver Nitrate or silver impregnated dressings such as Silverlon or Acticoat • Sulfamylon cream
Wound Care (cont) • Closed Method • Apply topical chemo and wrap with gauze, fluffs, kerlix • Assess for constriction; circulation checks
Emergent Phase (cont) • Elevate burned arms on pillows • Give pain meds 30 minutes prior to treatments • Wrap distal to proximal
Emergent Phase (cont) • Alteration in body temp (hypothermia) r/t loss of skin • Set thermostats at warm temp in room (~85 degrees) • Maintain body temp above 37 (98.6) degrees C; patient outcome on POC: • Patient will maintain body temp of 38 • (100.4)
Emergent Phase (cont) • Potential for injury r/t effects of stress response: • Stress diabetes What is the patho here??? • Curling’s ulcer (associated with burn trauma patients) • Gastroduodenal ulcer caused by increased gastric acid secretion
So which meds would nurse anticipate in the POC? Sliding scale and routine insulin sc H2 blockers for GI ulcer prevention: Pepcid, Protonix, Zantac