BURNS
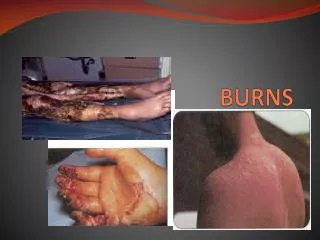
BURNS. James Taclin C. Banez M.D., FPSGS, FPCS. Etiology. Cutaneous burns caused by application of: Heat Cold Caustic chemical Electricity Depth of injury is proportional to: Temperature applied Duration of contact Thickness of skin. Etiology. Scald Burns:


BURNS
E N D
Presentation Transcript
BURNS James Taclin C. Banez M.D., FPSGS, FPCS
Etiology • Cutaneous burns caused by application of: • Heat • Cold • Caustic chemical • Electricity • Depth of injury is proportional to: • Temperature applied • Duration of contact • Thickness of skin
Etiology • Scald Burns: • Caused by hot water (most common burn in civilian practice) • 140F (60C) ---> deep partial of full thickness burns in 3 secs. • Exposed areas of skin burned less than clothed areas • Children and elderly has thinner skin • Immersion has longer contact • Scald burns from grease or hot oil are deep burns (400F/200C).
Etiology • Flame Burns: • 2nd most common mechanism of thermal injury. (house fire). • Flash Burns: • explosion of natural gas (petroleum) • clothing, unless it ignites, is protective • typically epidermal or partial thickness • Contact Burns: • Hot metals, plastic, glass or hot coals • Industrial accidents, motor vehicle • Are often 4th degree burns.
BURN SEVERITY Severity is related to: • Burn size • Burn depth • Part of the body burned
Burn Size: rule of 9 for adults For children: Lund-Browder burn chart child assumes adult once reach adolescence
Burn Depth: Determinant of mortality and long-term appearance and functional outcome. Burns leaving a part of the dermis leaves behind epithelium lined skin appendages Epithelial cells swarm from the surface of each appendages to meet adjacent swarming cells
The thickness of skin varies with age, sex and area of the body: • Epidermis is thickest (0.5cm) on palm & sole • Dermis varies from 1mm on the eyelids and genitalia to more than 5mm at the back. • Dermal atrophy >50y/o and skin appendages are less active.
Burn depth is dependent on: • Temperature of the burn source • Thickness of the skin • Duration of contact • Heat-dissipating capability of the skin (blood flow).
Classification of Burn According to Increasing Depth • Shallow Burns: • Epidermal Burn: (1st degree) • No blister • Erythema due to dermal vasodilation • Quite painful • 4th day injured epithelium desquamate – peeling (sunburn)
Classification of Burn According to Increasing Depth • Shallow Burns: • Superficial Partial-thickness: • Second degree • Includes upper layer of dermis • Characteristically forms blisters (fluid accumulation between epidermis and dermis). • If blisters are removed the wound is pink, wet, painful and blanch w/ pressure • Heal spontaneously < 3wks w/o functional impairment • Rarely cause hypertrophic scarring, but never completely match color of surrounding normal skin
Classification of Burn According to Increasing Depth • Deep Burns: • Deep Partial Thickness: (second degree) • Extends into the reticular layer of the dermis • w/ blisters but wound surface mottled pink and white color • Complains of discomfort rather than pain • Pressure applied --> capillary refill is slow or absent. • 2nd day wound is white and dry • If not excised & grafted heals in 3 to 9 wks w/ scarring • Joint function can be impaired
Classification of Burn According to Increasing Depth • Deep Burns: • Full Thickness: (third degree) • All layers of the dermis • Appear white, cherry red or black and may or may not have deep blisters • Leathery, firm and depressed compared w/ adjoining normal skin • Insensate • Develop a classic burn eschar, an intact dead and denatured dermis that separates after days or wks. • Heal only by wound contracture, epithelialization from the wound margin or skin grafting
Classification of Burn According to Increasing Depth • Deep Burns: • Fourth Degree: • Involves also the subcutaneous fat and deeper structures • Almost always have charred appearance • Electrical burns, contact burns, immersion burns and patients who are unconscious at time of burn
Those that will heal w/in 3wks are better treated by nonoperative wound care: • Shallow burns • State-of-the-art burn care involves early excision and grafting (E&G) of all burns that will not heal w/in 3wks: • Deep burns
Assessment of Burn Depth • Standard technique for determining burn depth: clinical observation of the wound • Other techniques to qualify burn depth: • Ability to detect dead cells or denatured collagen (biopsy, ultrasound, vital dyes) • Assessment of changes in blood flow (fluorometry, laser doppler & thermography) • Analysis of the color of the wound (light reflectance methods) • Evaluation physical changes, such as edema (MRI)
Physiologic Response to Burn Injury • Burn – inflammatory process involving the entire organism • Systemic Inflammatory Response Syndrome (SIRS): • Alterations of the metabolic, cardiovascular, gastrointestinal and coagulation systems • Resulting to hypermetabolism, increased cellular, endothelial and epithelial permeability • Often extensive microthrombosis
Physiologic Response to Burn Injury Burn Shock: • Complex process of circulatory and microcirculatory dysfunction that is not easily or fully repaired by fluid resuscitation. • Tissue trauma & hypovolemic shock releases local & systemic mediators ---> increase vascular permeability and microvascular hydrostatic pressure --->burn edema. • Histamine – causes increased vascular permeability by disrupting venular endothelial tight junction--> egress of fluids and proteins • Released by masts cells in burned skin • Serotinin – increases vascular resistance amplifying vascular effects of NE, histamine, angiotensin II
Physiologic Response to Burn Injury Burn Shock: • Eicosanoids – vasoactive products of arachidonic acid metabolism • Released in burn tissue; produced edema • Increases the level of Prostaglandin causing vasodilatation leading to increase bld flow and hydrostatic pressure ---> edema • Kinins (bradykinins) – inc. premeability • There is hypercoagulable and hyperfibrinolytic state
Pathophysiology of Burn Shock: • Hypovolemic etiology: • Decreased cardiac output • Increased extracellular fluids • Decreased plasma volume • Oliguria • In burn shock, resuscitation is complicated by obligatory burn edema • Maximal edema formations occurs between: - 8-12hrs in small burns - 12-24hrs in major burns
Pathophysiology of Burn Shock: • Changes in cellular level: • >30% burn; cell transmembrane potential ----> Na-K ATPase • Due to defective ATP metabolism
Physiologic Response to Burn Injury Metabolic Response to Burn Injury • Hypermetabolism: • > 100% REE (1.3x BMR) due to: • Increased heat loss from the burn wounds • Due to increased blood flow and skin loss • Increased beta-adrenergic stimulation • Increased catabolism of CHO, Lipids and CHON • Neuroendocrine Response: • Catecholamine massively elevated and major endocrine mediator of hypermetabolism in burn • Giving propranolol – diminish REE and O2 consumption
Care at the scene: Airway: CPR 100% O2 via a nonrebreather mask if there is any suspicion of smoke inhalation If unconscious or in respiratory distress ----> endotracheal intubation
Care at the scene: • Other injuries and transport: • assess other injuries; transport to nearest hospital • kept flat and warm and wrapped in clean sheet and blanket, NPO • IVF = lactated Ringer’s sol. at rate of 1liter/hr. in case of severe burns • Constricting clothing and jewelry shd be removed from burned parts due to local swelling begins
Care at the scene: • Other injuries and transport: • assess other injuries; transport to nearest hospital • kept flat and warm and wrapped in clean sheet and blanket, NPO • IVF = lactated Ringer’s sol. at rate of 1liter/hr. in case of severe burns • Constricting clothing and jewelry shd be removed from burned parts due to local swelling begins
Care at the scene: • Cold Application: • Cooling cannot reduce skin temperature enough to prevent further tissue damage • Cooling delays edema formation by reducing initial thromboxane production • Ice or cold water: • Never be used for it can lead to systemic hypothermia and associated cutaneous vasoconstriction can extend thermal damage
Emergency Care Emergency Room Care: • Primary rule for emergency physician is to ignore the burn • ABC: Search for other life- threatening injuries
Emergency Room Care: • Emergency assessment of inhalation injury: • Suspected in flame burns or anyone burned in an enclosed space • Rescuers are the most important historians • Signs of potentially serious airway injury • Hoarseness & expiratory wheezes • Copious mucus production and carbonaceous sputum
Emergency Room Care: • Emergency assessment of inhalation injury: • Decreased P:F ratio (Pao2:FIO2), is one of the earliest indicators of smoke inhalation. • 400-500 is normal • < 300 = impending pulmonary problem • < 250 = indication for endotracheal intubation • Fiberoptic bronchoscopy – can accurately assess edema of upper airway.
Emergency Room Care: • Fluid Resuscitation: • IV LR 1L/hr in adult 20ml/kg/hr in children • Foley catheter – UO/hr.: • 30ml/hr in adults • 1ml/kg/hr in children • After ascertaining the extent of the burn estimate the fluid needs: • Parkland formula: 4ml/kg/%burn (LR) • Modified Brooke: 2ml/kg/%burn (LR) • <50% TBSA use 2 large bore IV line >50% or other medical problems CVP >65% TBSA--> burn center • Use upper extremities as portals for IV
Use colloid formulas: Evans: NSS 1ml/kg/%burn 1ml/kg/%burn 2000ml D5W Brooke: LR 1.5ml/kg/%burn 0.5ml/kg 2000ml D5W Slater: LR 2L/24h Fresh frozen plasma 75ml/kg/24hr Colloid generates inward oncotic force to counteracts outward intravascular hydrostatic force. Other formulas estimating adult burn pt resuscitation fluid needs:
Emergency Room Care: • Tetanus prophylaxis: active/passive • Gastric decompression: NGT • enteral feeding ---> reduce Curling ulcers, prevents ileus and blunt catabolism • Pain control: IV opiates • Psychosocial care
Care of Burn Wound: • In transferring a pt, wound is minimally dressed in gauze; pulses distal to circumferential deep burns should be monitored • Escharotomy: • Edema formation--> vascular compromise---->permanent neuromuscular & vascular deficits. • Skin color, sensation, capillary refill and peripheral pulses assessed hourly • S/Sx warrants escharotomy: • Cyanosis • Deep tissue pain • Progressive paresthesia • Progressive decrease or absence of pulses • Sensation of cold extremities
Respiratory distress due to deep circumferential burn wound of the thorax Local anesthesia is not needed; but IV opiates or anxiolytics is given.
Carbon Monoxide Poisoning: • Majority of house fire deaths • CO2 is colorless, odorless and tasteless gas w/ affinity to Hgb 200x that of 02. • Mechanisms of interfering O2 delivery: • Prevents reversible displacement of O2 on the Hgb molecule • COHg shifts the O2-Hg dissociation curve to the left. • CO2 binds to reduced cytochrome a3, causing less effective intracellular respiration • CO bind to cardiac and skeletal muscle, direct toxicity • CO act in CNS causing demyelination causing neurologic symptoms.
Carbon Monoxide Poisoning: • Symptoms: • Headache, N/V, loss of manual dexterity • Weak, confused and lethargic • Coma • CO reversibly bound to the heme: • Room temp = half-life (t1/2) of COHb is 4hrs • 100% O2 = t1/2 is reduced to 45-60mins • Hyperbaric O2 at 2atm. = t1/2 30mins • Hyperbaric )2 at 3atm. = t1/2 15-20min • Tx: 100% oxygen via a nonbreather face mask
Thermal Airway Injury: • Most of the heat in burning room is dissipated in the oropharynx, nasopharynx and proximal tracheobronchial tree due to: • Oropharynx and nasopharynx provide an effective mechanism of heat exchange due to: - large surface area - associated air turbulence - mucosal fluid lining that acts as a heat reservoir. • Sudden exposure to hot air typically triggers reflex closure of the vocal cords
Thermal Airway Injury: • Greatest risk: • Explosion • Burns of face and upper thorax • Unconscious in a fire • Edema ---> upper airway obstruction • Presence of intraoral and pharyngeal burns indication ---> endotracheal intubation • Tube is placed until edema subsides • Steroid has no role in tx upper airway edema in burns.
Smoke Inhalation: • Product of combustion (hydrogen cyanide) • Wheezing and air hunger early manifestations of inhalation injury: • Classical findings in pulmonary function test: • Decreased functional residual capacity • Decreased vital capacity • Evidence of obstructive disease w/ reduction in flow rates • Increase in dead space • Rapid decrease in compliance • Concomitant cutaneous burn releases mediators (Prostaglandin, thromboxane, and reactive O2 intermediates) that can aggravate pulmonary injry. • w/o associated cutaneous injury, mortality from isolated inhalation injury is quite low.
Diagnosis: • Anyone w/ flame burn sustained in an enclosed space is assumed to have inhalation injury until proven otherwise. • Hoarseness, stridor, edema or soot impaction • Chest auscultation for wheezing or rhonchi suggesting injury to distal airway • Level of consciousness associated w/ decreased w/ hypoxia, CO poisoning or cyanide poisoning • Testing for the presence of neurologic deficits associated w/ CO. • Copious mucus production and carbonaceous expectorated sputum • Al elevated COHb or any symptoms of CO poisoning are presumptive evidence of associated smoke inhalation • Earliest indication of smoke injury is decreased P:F ratio. • Routine use of fiberoptic bronchoscopy
Treatment: • Upper Airway: • Rapid endotracheal intubation due to oropharyngeal/laryngeal edema. • Ability of adult pt to breathe around the tube w/ the cuff deflated is an indication for tube removal. • Tx of postextubation stridor: • Administration of nebulized racemic epinephrine and helium-oxygen mixtures • Steroids are never used.
Treatment: • Lower Airway and alveoli: • Overall treatment for smoke inhalation is supportive w/ the goal being maintenance of adequate oxygenation and ventilation until the lungs heal. • Mild cases are treated w/ humidified O2, vigorous pulmonary toilet, and bronchodilators as needed. • If w/ atelectasis, positive end-expiratory pressure is useful to increase FRC, increasing oxygenation.
Treatment: • Lower Airway and alveoli: • High frequency percussive ventilation (HFPV) provide superior oxygenation at a lower FIO2, w/ lower airway pressures than conventional mechanical ventilation. This enhanced clearance of bronchial secretions • Cricothyroidotomy for danger imminent obstruction and unsuccessful endotracheal intubation. This is later converted to tracheostomy • Prophylactic antibiotics are indicated w/ inhhalation injury, which is a chemical pneumonitis. • Steroids are contraindicated due to septic complications and higher mortality rate
Shallow burns healed w/in 3 wks while deep burns healed over many weeks if infection was prevented • For deeper wounds rather waiting for spontaneous separation, the eschar is surgically removed and closed via grafting techniques and/or immediate flap procedures (E&G) • Early E&G has reduced burn mortality more than any other intervention. It decreases the number of painful debridements required. Immunosuppression and hypermetabolism associated w/ burns is ameliorated
NOTE: • His notes only cover up to page 204 in schwartz. • READ!!! Pg. 205-217 • Good luck