BURNS
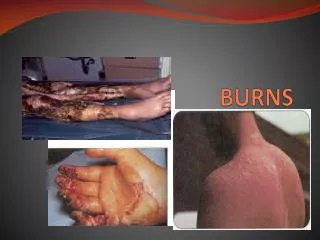
BURNS. Burns. can be caused by: thermal (heat) injury burns – dry heat (flames) scalds – wet heat: hot liquids and vapour frostnips – completely reversible cold injury Frostbites – completely irreversible cold injury chemical injury (corrosive substances) electrical injury


BURNS
E N D
Presentation Transcript
Burns can be caused by: • thermal (heat) injury • burns – dry heat (flames) • scalds – wet heat: hot liquids and vapour • frostnips – completely reversible cold injury • Frostbites – completely irreversible cold injury • chemical injury (corrosive substances) • electrical injury • radiation injury (X-rays, sun)
Classification and assessment of burns • Depth of the burn • Extent of the burn • Location of the burn • Complicating factors (age, respiratory involvement, associated medical or traumatic conditions)
Depth of burns Superficial burns (1st degree) • involve only the outer layer of the skin • redness, swelling, tendreness, pain • examples: mild sunburn, scald produced by a splash of hot liquid • heal well if prompt first aid is given • do not require medical attention unless exstensive
Depth of burns Partial – thickness burns – 2nd degree • the skin looks raw with blisters formation • heal well but > 50% of the body surface can be fatal
Depth of burns Full thickness burns – 3rd degree • all layers of the skin are burned • affected nerves, muscles and fat • the skin may appear pale, waxy, black • any size of that type need medical attention as quickly as possible
EXTENT OF BURNS The area of burn gives an approximate indication of the degree of shock that will develop. • any II0 burn of 1% bs (area of patient hand) must be seen by doctor • II0 burn of 9% bs or more can cause shock • every III0 burn of any size requires hospital treatment
Location of burns Burns to the special areas are more critical: • the face – often accompanied by respiratory tract involvement, possibility of oedema • the perineum and genitalia – prone to infection as a result of contamination from fecal bacteria • the feet and hands – special handling to avoid contractures and scarring that will restrict future function
Complicating factors • inhalation injuries – damage to the airways and lung themselves • age of the patient – adults > 55 y. and children < 5 y. are considered at increased risk • associated conditions – preexisting disorders (lungs, heart, diabetes) • burn severity
Treatment of burns • stop the burning process + cooling (cold water for at least 10 minutes) • remove the patient from the smoky environment • provide supplemental oxygen (reversing the effects of carbon monoxide) • treat the patient for shock • the blisters should be left intact (barrier to infection) • prevent infection – use non-fluffy material for dressing – kitchen film, clean plastic bag • transport the patient to the appropriate facility
TREATMENT OF BURNSThe priority is to cool the injury - use cold liquid for > 10 min.While cooling monitor vital signs
TREATMENT OF BURNSDRESSINGto protect from infection cover with non-fluffy material (plastic kitchen film, a clean plastic bag)
Burns CHEMICAL • the signs of chemical burns develop slowly. • DO NOT delay starting treatment by searching for an antidote. • flood the affected area with water to disperse the chemical and stop the burning process (> 20 min.) SUNBURN • place the casualty in the shade, cool by cold water, give cold water to drink, administer aspirin
Electrical burns • electricity transvering the body is converted to heat that burns the tissues in its path • death can result from passage of currnet through vital organs • electrical current passing through the body follows an internal path of least resistance (skin, bones > muscles > vessels and nerves) • current can enter and exit at relatively small surface areas that don’t correspond to the internal injuries
Types of bleeding • arterial - pulsing, strong, haemorrhagic shock can occur • venous - depends on the size of vein, serious from varicose veins • capillary - not very intensive, from the surface of the skin, depends on what the surface is
Severe external bleeding • raise and support the injure limb over the level of the casualty’s heart • apply direct pressure over the wound with your fingers or palm over a sterile dressing or clean pad (min. 10 minutes) • living a pad apply sterile dressing and bandage firmly but not so tightly to impede the circulation
INDIRECT PRESSURE PRESSURE POINTS the place where the main artery runs close to the bone. Pressure at these points will cut the blood supply to the limb. It must be applied for longer than 10 minutes. DO NOT use a tourniquet. It can make the bleeding worse and can result in tissue damage and gangrene.
Foreign bodies in minor woundspick off or rinse with cold water small piecesDO NOT try to remove object trapped in the wound strongly
Before applying bandages: • Explain to the casualty what are you going to do, and keep reassuring him. • Make the casualty comfortable, in sitting or lying position, if possible. • Keep the injured part supported. The casualty may be able to do this for you. • Always work in front of the casualty, and from the injured site where possible.
When applying bandages: • Apply bandages firmly enough to control any bleeding and hold a dressing in place, but not so tightly as to impede the circulation. • Leave fingers and toes on a bandaged limb exposed, if possible, so that you can check the circulation afterwards. • Ensure knots do not hurt the casualty, do not knot over bony areas.
Recognition of impaired circulation • Pale, cold skin on the hand or foot • Later, a dusky gray/blue appearance to the skin • Tingling or numbness • Inability to move the affected part
Checking for impaired circulation • Press one of the nails, or the skin of the hand or foot, until its pale. On releasing the pressure, the color should quickly return. If the nail-bed or skin remains pale, the bandage is too tight.
Checking for impaired circulation • Loose tight bandages by unrolling just enough turns for warmth and color to return to the extremity. The casualty may feel a tingling sensation. Reapply the bandage if necessary.
Securing roller bandages • Bandage clips • Adhesive tape • Safety pins
Securing roller bandages • After applying a roller bandage, leave enough of the end free to allow it to pass around the limb once and tie a knot. • Cut down the center of the loose end, and tie a knot at the bottom of the split. • Pass the ends once around the limb, one in each direction and tie them in a knot.
Injuries to the lower limb • Your aims are: • To immobilize the lower limb • To arrange urgent removal to the hospital
Injuries to the lower limb • Lay the casualty down. Ask a helper to steady and support the limb by holding it above and below the injury. • Gently straighten the lower leg and apply traction at the ankle, pulling steadily in the line of the limb. • Dial for an ambulance. • Gently position the casualty’s sound limb alongside the injured one.
Injuries to the lower limb • Insert padding between the tights, knees and ankles to prevent bandage-tying displacing the broken bone. • Gently slide two bandages under the knees and put them above and below the fracture. Position another bandages at the knees and the ankles. • Tie the bandages around his ankles and knees. Then tie the bandages above and below the fracture.
Injuries to the lower limb You can also use a wooden leg splint, walking stick, ski-stick, broomstick etc reaching from the armpit to the foot against the injured side and secure it with the broad-fold bandages at the chest and the pelvis, and hen at the legs. Do not bandage directly over the fracture.
When bandaging to immobilizea limb: • Make sure there is padding between the limb and body, or between the legs, especially around the joints. Use towels, cotton wool, or folded clothing, and insert the padding before tying the bandages. • Tie knots at the front of the body on the uninjured side, avoiding bony areas. If both sides of the body are injured, tie knots in the middle of the body.
Scalp bandage • apply gentle pressure to the wound with a flat hand • begin the head bandage by anchoring the bandage below the occipital protuberance
Scalp bandage • circle the head completely once or twice • begin to traverse the bandage back and forth across the top of the head until the area with dressing is completely covered • secure the bandage in place by circling the head once or twice and taping the bandage in place
Slings Slings can be made from triangular bandages, or any square metre of strong cloth, cut or folded diagonally. There are two different types of slings: • arm slings are used to support injured arms or wrists, or to take the weight of the arm off a dislocated shoulder. • elevation slings are used to support the arm in cases of collar bone or shoulder injuries. They can also be used in cases of hand injuries, as they help to control bleeding and reduce swelling because the hand is raised then.
Applying an arm sling • Place the bandage between the arm and the chest. Pull one end up around the back of the neck to the injured side.
Applying an arm sling • Bring the lower end of the bandage up over the casualty’s forearm to meet the other end at the shoulder.
Applying an arm sling • Tie a knot at the hollow over the collar bone on the injured side, and tuck the ends underneath.
Applying an elevation sling • Place the arm on the affected side across the chest, with the fingertips touching the opposite shoulder.
Applying an elevation sling • Drape the bandage over the casualty’s arm, with one end over the shoulder and the point well beyond the elbow on the injured side.
Applying an elevation sling • Ask the casualty to release her arm. Supporting the arm, tuck the base under her forearm and behind her elbow.
Applying an elevation sling • Bring the lower end up diagonally across her back to meet the other end at the shoulder. Tie a knot in the hollow above the casualty’s collar bone. Tuck the ends under the knot.
Applying a roller bandage • Place the end of the bandage below the injury and, working from the inside of the limb outwards, make two straight turns with the bandage head.
Applying a roller bandage • Make a series of spiral turns, working up the limb. Allow each successive turn to cover between a half and two-thirds of the previous layer.
Applying a roller bandage • Finish off with one straight turn, and secure the end.
Elbow and knee bandage • Support the injured arm in a semi-flexed position. If this is not possible, support the arm in the position most comfortable for the casualty.
Elbow and knee bandage • Place the tail of the bandage on the inside of the elbow, and pass the bandage around the elbow 11/2 times, so that the elbow joint is covered.
Elbow and knee bandage • Take the head of the bandage above the elbow to the upper arm, and make one turn, covering half of the bandage from the first turn. Take the head of the bandage under the elbow to just below the joint, and make one turn around the lower arm, covering half of the first straight turn.
Elbow and knee bandage • Continue to alternate these turns, steadily extending the bandaging by covering only between half and two-thirds of the previous layer each time. Make two straight turns to finish off, and secure the end.