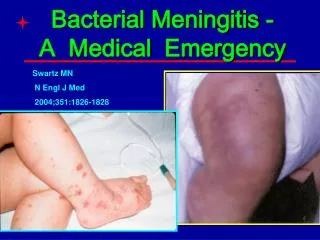
Bacterial Meningitis
Bacterial Meningitis. Ziad Elnasser, MD, Ph.D. Anatomical considerations. CNS parts. Blood brain barrier. CSF and its circulation. Hydrocephalus. Routes of infection. Blood borne. Occult or overt. Remote focus. Venous spread. Direct. Congenital. Surgery complications.


Bacterial Meningitis
E N D
Presentation Transcript
Bacterial Meningitis Ziad Elnasser, MD, Ph.D
Anatomical considerations • CNS parts. • Blood brain barrier. • CSF and its circulation. • Hydrocephalus.
Routes of infection • Blood borne. • Occult or overt. • Remote focus. • Venous spread. • Direct. • Congenital. • Surgery complications.
General characteristics • G –ve diplococci, size variations. • Polysaccharides capsule. • Colonial morphology. • Growth conditions and media. • Carbohydrates fermentation. • Oxidase positive. • Significance of iron.
Antigenic structure • Capsular polysaccharides. • Quellung reaction, group A and C. • 13 serotypes: A, B, C, D, X, Y, Z, E, W135, H, I, K and L. • A, B, C, X, Y, Z, W135, and L has been purified. • Group C divided into Neuraminidase R or S. • Serogrouping and antibiotics resistance? • Group B not immunogenic.
Noncapsular Cell wall Antigens • Like other G –ve bacteria. • Lipo-oligosaccharide (12 serotypes). • Similar to human Glycosphingolipid Antigens. • Lipo-oligosaccharides as future vaccines. • OMP typing. • Classification based on Serotyping, OMP and Lipo-oligosaccharides.
Pili • Phase and antigenic variation. • Attachment to nasopharyngeal cells. • Colonies of Piliated and nonpiliated are the same not as that of Gonococci.
Pathogenesis • Nasopharyngeal surface. • Ciliated or nonciliated. • Mucus. • Pili and attachment to MCPs (CD46). • Opa and Opc role. • Only non encapsulated strains invade? • Actin rearrangement and porin protein. • IgAase and Pil C role and BB barrier.
Immune response • Group A antigen and Bacillus pumilis. • E. coli K1 antigen and Group B. • Neonatal tissue and group B. • Some times not protective. • IgAase only in pathogenic strains.
Carrier state • Presence of the meningococci in healthy individuals. • Parameningococci. • Carrier state and epidemic status, >20%. • Carrier to carrier via respiratory route. • Normal flora role. • Group B is the most common (9.6months). • Invasion and newly infected patients. • Upper respiratory tract infection and carriage.
Epidemiology • Worldwide epidemics. • 5 – 19 years old during epidemic. • Fatality rate 2 – 10% and in septicemia up to 70%. • Low socioeconomic status and poverty. • Serotypes and different epidemic potential. • School children, military recruits and medical personnel.
Clinical manifestations • Ranges from mild fever to septicemia and fulminant death. • Bacteremia without sepsis, upper respiratory tract infection. • Meningococcemia, leukocytosis, skin rash, headache and hypotention. • Meningitis with or without septicemia. • Meningoencephalitic manifestation. • Children vs adults.
Laboratory Diagnosis • CSF and Blood. • Synovial, pleural, petechial skin and mucosal lesions and pericardial. • Chemical and cytological examination. • CIE, latex agglutination, coagglutination. • Lactate dehydrogenase and neuraminidase detection. • PCR value if antibiotics were used.
Treatment • Antibiotics reduced mortality and supportive care improved prognosis. • Sulfonamides. • Penicillin. • Chloramphenicol. • First generation cephalosporins?. • Second and third generation cephalosporins. • Value of early treatment.
Supportive care • Treat complications caused by LPS. • TNF alpha and other cytokines as indicators of shock. • Complement level. • Recombinant proteins. • Steroids? Low dose. • Heparin? • Plasmin activator with fibrinolysis for DIC.
Chemoprophylaxis • Sulfonamides reduced the carrier state. • Penicillin proved to be ineffective. • Rifampin and minocycline. • Ciprofloxacin. • Ceftriaxone. • House hold contacts, medical personnel, nursery schools, military barracks
Immunoprophylaxis • Capsular polysaccharides A and C. • Erythema and irritability in some. • Not effective before 24 months of age. • Day care centers. • Hyporesponsiveness. • Now quadrivalent of A, C, Y and W135 is avialable. • Detoxified LOS and OMP, Capsule protein conjugate, anti-idiotype antibodies.
CRYPTOCOCCOSIS • Cryptococcus neoformans. • Yeast , large capsue unique, polysaccharide • Urease positive. • Bacterial like colonies. • Pigeon and birds droppings in soil. • No human to human transmission.
PATHOGENESIS • Inhalation of yeast or conidia. • Minimal signs and symptoms. • CNS is the primary target. • Common complication of AIDS. • Phagocytosis? • Humoral and CMI role.
CLINICAL MANIFESTATIONS • Meningitis, skin, pneumonia. • Slow insidious onset. • Headache, irritability, dizziness and behavioural changes. • Seizures, cranial nerves, papillidema, and dementia. • In AIDS 5 - 15% becomes infected.
DIAGNOSIS • CSF pleocytosis, lymphocytes predominance, Sugar, protein. • Microscopy, negative staining. • Culture, urease. • Serology.
TREATMENT • Amphotericin B + Flucytosine. • Fluconazole. • Relapse is a problem, chronic. • Residual neurological damage.
Viral Meningitis • Self limiting to severe. • Meningitis vs encephalitis and clinical course. • Viral infections in the immune suppressed. • Slow viral infections. • Unconventional infections.
Aetiological agents • Acute Aseptic Meningitis Syndrome • Mumps. • Coxsakie. • Echo. • HSV-2 • HIV • Polio • Lymphocytic choriomeningitis virus.
Acute lymphocytic pleocytosis in the CSF. • No involvement of the brain paranchyma. • Normal sugar and slight protein increase. • Clinical course is usually mild. • Trimethoprim, Ibubrufin, Carbamazipine. • IV Immunoglobulin injection. • Treatment is supportive.
Acute encephalitides • Parenchymal affection. • Like viral meningitis but more severe symptoms, seizures to coma. • Togaviruses, mosquitoes, summer to fall. • St. Louis encephalitis. • Eastern Equine Encephalitis. • Western Equine Encephalitis. • California Encephalitis. • Supportive care.
HSV-2 some times HSV-1. • Acute widespread necrotizing infection of the newborne. Cervical infection and the baby. • Very high mortality or sever retardation. • HSV-1 and cold sores, frontal and temporal. • Acyclovir is effective mortality drops from 70 to 40%. • Steroids use.
Viral infections in the immune suppressed • PML and the JC virus. • Chronic demyelinating disease. • Hodgkin's, Lymphoma, Leukemia and HIV. • CSF studies are completely normal. • HIV and AIDS. • Opportunistic infections. • Double infection.
Slow Viral diseases • SSPE and mealses. • PRPE and Rubella. • Unconventional Agents: • Cretzfeldt-Jacob disease (prog. Dementia). • Kuru. • Gerstmann–Straussler-Scheinker Syndrome. • Familial Fatal Insomnia. • Bovine Spongiform encephalopathy. • Scrapie, Transmissible Mink encephalopathy, chronic wasting disease.