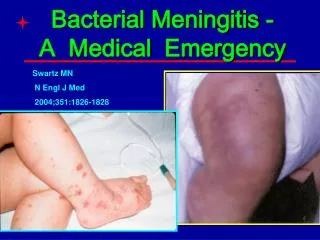
Bacterial Meningitis
Bacterial Meningitis. Objectives . To define bacterial meningitis To discuss the causative pathogens To discuss clinical presentation To discuss diagnosis and lumbar puncture To discuss management including antibiotics and dexamethasone To discuss outcomes and follow up


Bacterial Meningitis
E N D
Presentation Transcript
Objectives • To define bacterial meningitis • To discuss the causative pathogens • To discuss clinical presentation • To discuss diagnosis and lumbar puncture • To discuss management including antibiotics and dexamethasone • To discuss outcomes and follow up • To discuss Meningococcal disease • To discuss prevention
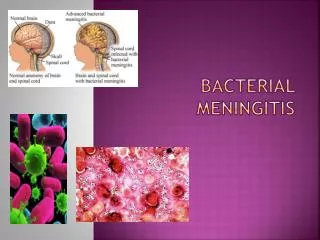
What is meningitis ? • Meningitis • Encephalitis • Meningoencephalitis
Bacterial Pathogens • Depends on Age • Depends on underlying conditions • Depends on vaccination status • Depends on Geographical location
Bacterial Pathogens Neonatal period • Group B Strep. 49% • E.Coli 18% • Listeria 7% • Misc. Gram. Neg. 10% • Misc. Gram. Pos. 10%
Bacterial Pathogens Older than 1 month • Neiserria Meningitidis(Meningcoccus) • Strep. Pneumoniae (Pneumococcus) • H.influenzae ( Now rare )
Bacterial Pathogens V-P Shunt • Staph. Epidermidis • Staph. Aureus • Coliforms Post Head injury • Strep. Pneumoniae most common if CSF leak ( Consider s.aureus/Pseudomonas)
Symptoms of Meningitis Depends on Age Older Child • Fever, Chills, vomiting, photophobia & severe headache • Seizures Younger Child • More subtle – poor feeding, drowsy, quiet, ‘Not herself’
Clinical Signs of Meningitis Signs of infection: Fever, pallor. Raised ICP: Elevated BP with decreased Heart rate. Papilloedema Nuchal Rigidity: Neck stiffness – not soreness
Clinical Signs of Meningitis Kernigs: “If one attempts to extend the patient’s knees one will succeed only to an angle of approximately 135°. In cases in which the phenomenon is very pronounced the angle may even remain 90°.” Brudzinskis: With the patient lying on the back: if the neck is forcibly bended forward, there occurs a reflexive flexion of the knees.
Role of Lumbar Puncture (LP) • CSF analysis and culture is the definitive method of diagnosis • Identifying pathogen allows rationalisation of antibiotic treatment and collection of epidemiological information • Definitive diagnosis allows better outcome prediction.
Role of Lumbar Puncture When to LP? • When meningitis is suspected • When its safe ! • ? Role of CT • Sterilisation of CSF after antibiotics • Molecular techniques
Contraindications to Lumbar Puncture Signs of cerebral herniation • GCS < 8 • Abnormal pupillary signs • Abnormal tone / posture • Papilloedema Focal neurological signs Cardiorespiratory compromise Obvious signs of Meningococcaemia
Management Airway Breathing Circulation Drugs
Circulation How much fluid? • Fluid restriction no longer recommended in meningitis • Consider SIADH in later management • Massive fluid resuscitation may be required for meningococcal sepsis
Antibiotics Choice depends on • Causative Pathogen • Resistance of Local pathogens • Penetrance of CSF
The role of Steroids • Dexamethasone now recommended for all types of bacterial meningitis. • Improved neurological outcome – especially hearing. • Must be given early – with initial antibiotics. • Some concern over use with resistant pneumococcus
Complications Early & Late include • Circulatory collapse – not just meningococcal • Focal neurological abnormalities • Hydrocephalus • Brain abscess • Seizures
Outcome from Bacterial Meningitis Mortality - Less than 10% • Reports of less than 2% in infants and children • Reports of up to 30% in Neonates and Adults Morbidity – 15% (10-30%) • Hearing • Seizures • Learning problems • Lower IQ when compared with sibs
Meningococcal Disease • May present as meningitis or as sepsis (Meningococcaemia) or both. • Significant differences in management depending on presentation. • Endotoxins trigger “Sepsis Syndrome” • Meningococcaemia may cause profound shock and may require significant fluid resuscitation. • Also associated with Disseminated intravascular coagulation (DIC). • Mortality reduced by early recognition and administration of IM Penicillin
Prevention of Bacterial Meningitis Vaccination • H.Influenzae – incidence decreased by > 99% • Meningococcal A & C – Problems with B • Polyvalent pneumococcal • New vaccines Perinatal Screening • HVS for Group B Strep. • Antepartum penicillin Chemoprophylaxis • House hold contacts of children with meningococcus or H. influenza • Usual treatment Rifampicin for 2/7
Conclusions • Significant infection • Pathogen usually depends on age of the child • Choice of antibiotic is based on the likely pathogen • Meningococcal disease may manifest as meningitis or sepsis – separately or combined • Prevention is still better than cure
References • Bacterial meningitis in children Xavier Sáez-Llorens, George H McCracken Jr The Lancet. Volume 361 Issue 9375 Page 2139 • Diagnosis and treatment of bacterial meningitisH El Bashir, M Laundy, and R BooyArch. Dis. Child., Jul 2003; 88: 615 - 620.