Immunizations
Immunizations . Childhood and Adolescent Jan Bazner-Chandler CPNP, MSN, CNS, RN. What Immunization Is. Immunization is the process by which a subject is rendered immune or resistant to a specific disease Natural exposure – contact with the agent

Immunizations
E N D
Presentation Transcript
Immunizations Childhood and Adolescent Jan Bazner-Chandler CPNP, MSN, CNS, RN
What Immunization Is • Immunization is the process by which a subject is rendered immune or resistant to a specific disease • Natural exposure – contact with the agent • Artificial exposure – parts of the infectious agent or inactivated version is given for the purpose of becoming immune to the disease agent it causes.
Childhood Immunization • Childhood immunization schedule American Academy of Pediatrics • http://www.cispimmunize.org/ • Download children age 0 - 6 • Download children age 7 - 18
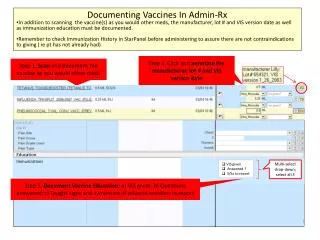
Hepatitis B (HepB) Vaccine • All infants should receive the first dose soon after birth or before hospital discharge. • Second dose should be given at least 4 weeks after the first • Third dose 16 weeks after the first dose and at least 8 weeks after the second dose • Infants born of HBsAg-postive mothers should receive first immunization within 12 hours of birth as well as HBIG.
Diphtheria, Tetanus, Acellular Pertussis • DTaP • Given at 2, 4 and 6 months • 4th dose between 15 and 18 months • Last DTaP at the 4-6 year pre-K check up • 1st Tdap at age 11-12 years or at least 5 years from last DTap • Every 10 years after that
Polio • Injection form at 2 months, 4 months after 6 months and at kindergarten check-up • Oral not given due to shedding in stool.
Haemophilus Influenza Type b • Hib • Given at ages 2 and 4 months • Last dose at 12 months • Any child entering child care or pre-kindergarten under age 5 years would be required to have Hib. • Not a standard immunization for children born outside the USA
Measles, Mumps, Rubella • MMR • Two doses: • 1st 12 months or older • 2nd dose kindergarten visit • If no record of second dose it should be given at 11 to 12 year old visit • May develop a rash a week to ten days after immunization • Not immunized against wild strain – exposure would bring milder case
Varicella • Chicken pox – recommended at 12 months and second dose at 4-6 years or kindergarden visit • Susceptible children over 13 years would receive two doses at least 4 weeks apart
Pneumococcal Vaccine • PCV - Prevnar • Recommended for all children 2 to 23 months and certain populations up to 59 months • Asthma • Sickle cell anemia • Cystic fibrosis • 2, 4, 6 and 4th dose after 12 months of age
Human Papillomavirus • HPV is the most common sexually transmitted virus • 40 types of HPV • Spread through sexual contact • Can cause cervical cancer • Can also cause genital warts
Human Papillomavirus • HPV series • Recommended for all girls 11-12 years • Can be given as young as 9 years • Get HPV before first sexual contact • 1st dose • 2nd dose 2 months after 1st dose • 3rd dose 6 months after dose one
HPV • Contraindications: • Allergy to yeast or reaction to first immunization • HPV will not help if already infected
Meningococcal • Meningococcal disease is a serious illness • Leading cause of bacterial meningitis in 2 – 28 year old in USA
Meningococcal polysaccharide Vaccine • MPSV4 • Prevents 4 types of meningococcal diseases – 2 out of 3 of the most common strains seen in the US
Recommendations • MCV4 recommended for all children at their routine preadolescent visit (11 – 12 years) • College freshmen living in dorms • U.S. military recruits • Traveling to Africa • Persons exposed to meningitis outbreak
Influenza (Flu) Vaccine • “Flu shot”: Inactivated vaccine containing the virus • Approved for infants older than 6 months • Nasal spray flu vaccine: live, weakened flu viruses • Approved for children over 5 years to 49 years.
When to get Flu Vaccination? • October or November yearly
Contraindications to Flu Vaccine • Children with severe allergy to chicken eggs. • Severe reaction to influenza vaccination in the past. • Less than 6 months of age. • Children who have developed Guillain-Barre syndrome after previous immunization. • Do not give if child has moderate to severe illness with fever until a later date.
Premature Infants • AAP currently recommends that all premature infants receive full dose immunizations at the same chronologic age as term infants even if hospitalized • Contraindications include: significant febrile seizure, active seizure disorders, encephalopathy (DTaP) • Infants with BPD or RAD should receive influenza immunizations • Infants with congenital heart and premature infants immunization against RSV.
Premature continued • Hepatitis B may be deferred until discharge unless mother is Hep B positive • OPV should not be given in NICU • Do NOT dilute dosages • Usually given when they reach at least 2 kg or 4.4 pounds
To Immunize or Not to Immunize • Children on antibiotics • Children with minor illness – otitis, cough, diarrhea, sore throat, low grade fever • Children with mild allergies • Breast feeding infants • Children with pregnant household contacts
True Contraindications • True allergic response • Rash or hives after previous vaccination • Allergy to eggs or egg products should not be given influenza vaccination • Allergic to streptomycin should not be given IPV or influenza vaccination
Reactions to Immunizations • Fever greater than 103, shock or collapse, or inconsolable crying for greater than 3 hours. (DTaP) • Low grade fever, fussiness, and soreness at injection site are not reasons to prevent further vaccinations • Mild rash or fever may occur 10 days to 2 weeks after MMR or Varicella
Interventions • Tylenol every 4 hours for fussiness or low grade fever • Warm bath • NO ASPIRIN • NO Motrin for infants under 6 months of age • AAP recommends Tylenol for all ages due to confusion in dosing.
Adolescents • Hepatitis A (recommended only) • Pneumococcal if they have any chronic disease: heart, sickle cell disease, cystic fibrosis, diabetes, or organ transplant or receiving chemotherapy • Hepatitis B • MMR: second booster • D Tap • Varicella if no reliable history or negative titers • Meningococcemia for all college freshman and all military • Influenza yearly
Hepatitis A • Recommended for children and adolescents living in selected states or regions and for certain high risk groups • This would include California, Texas, and Arizona • 2 doses 6 months apart
Live Vaccines • MMR and Varicella • Pregnancy • HIV + • Immunodeficiency • Chemotherapy: not given until 6 months after treatment is completed.
L.A. Unified Recommendations • Complete health and immunization record • All new students must have written results of a PPD test for tuberculosis within 12 months • If Manoux test is positive a chest x-ray is required • Treatment is recommended unless the child has some immune suppressed condition.
PPD Waiver • I hear by request exemption of the child from the tuberculosis assessment requirement for school / childcare entry because this is contrary to my beliefs. I understand that should there be cause to believe that my child is infected with active TB or should there be a tuberculosis outbreak, my child may be temporarily excluded from school.
Pre-school and Child Care • Pre-kindergarteners must be immunized against Haemophilus influenza type B or Hib. • This is not a standard immunization for children born outside the United States • Hib would not be required for a child over 5 years of age.
Kindergarten • Second MMR: Measles, Mumps, Rubella • Hepatitis B • Hepatitis A in high risk areas • D Tap: tetanus, diphtheria, pertussis
Communicable Diseases • Chicken pox (varicella) • Measles (Rubeola) • Pertussis (Whooping Cough) • Rubella (German Measles) • Scarlet Fever • Mumps
Varicella • Agent: varicella zoster virus • Incubation: 10 – 14 days • Transmission: respiratory • Period of communicability: 2 days before eruption of vesicles until lesions crusted. • Prodromal phase: slight fever, malaise, pruritic rash; macular to papular to vesicular.
Varicella • Communicability: children who have “chicken-pox” are infectious for two days before the vesicles erupt until all vesicles are crusted over.
Management of Varicella • Isolation • Skin care: tepid bath, calamine lotion, clip finger nails. • Keep from scratching • Antihistamines for itching - Benadryl • No ASA – acetaminophen only. • Varicella vaccine now available.
Measles or Rubeola • Agent: Virus • Transmission: respiratory, blood and urine • Incubation period: 10 to 20 days • Period of Communicability: 4 days before and 5 days after rash appears. • Prodromal stage: fever, cough, conjunctivitis, Koplik spots.
Rubella or German Measles • Agent: Rubella virus • Source: nasopharyngeal secretions; secretions in blood, stool, and urine. • Transmission: direct contact. • Incubation period: 14 to 21 days • Period of communicability: 7 days before to 5 days after appearance of rash.
Rubella • Rash first appears on face and rapidly spreads downward • Isolate from pregnant women • TORCH – affects fetus
Mumps In mumps the parotid glands swell and obscure the angle of the jaw.
Mumps • Disease caused by a virus that spreads through saliva and infects many parts of the body especially the parotid salivary gland. • Incidence has decreased to about 1,000 per year. • Two potential complications: encephalitis and orchitis (inflammation of testicle)
Pertussis (Whooping Cough) • Agent: Bordetella Pertussis • Source: Respiratory • Transmission: droplet spread or contact with contaminated article. • Incubation period: 10 days • Period of communicability: before onset of paroxysms to 4 weeks after onset.
Interventions • Erythromycin for the child and all contacts • Very dangerous for the neonate – most often the contact is an adult with a chronic cough • May led to hospital admission – ventilator assist
Scarlet Fever • Caused by group A Streptococcus • Rash is usually seen in children under age 18 years. • Rash appears on chest and abdomen – feels rough like a piece of sandpaper • Redder in the arm pits and groin area. • Rash lasts 2-5 days • After rash disappears fingers and toes begin to peel • Face is flushed with a pale area around the lips.