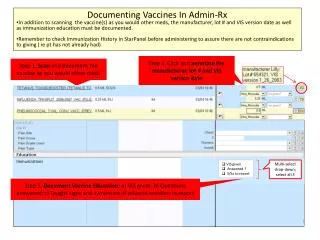
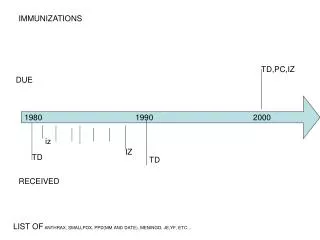
Adolescent Immunizations
This document highlights the critical need for improved adolescent immunization rates in the U.S., with specific focus on Utah and Tri-County areas. While infant immunization rates are commendable, adolescent vaccines such as Tdap and HPV show concerning gaps. The importance of protecting teenagers against serious diseases including pertussis and HPV, which is linked to various cancers, is emphasized. Data from recent years reveals alarming trends in HPV infections among teens. The need for proactive vaccination strategies to prevent future health crises is crucial.


Adolescent Immunizations
E N D
Presentation Transcript
Adolescent Immunizations Bill Cosgrove, MD FAAP Tri-county Immunization CoalitionApril 23, 2114
Adolescent Immunizations Credentials: Chair of Immunization Committee, UTAAP (since 1987) Chair, Utah Every Child By Two Immunization Coalition (in abeyance) Member, Steering Committee USIIS Member, Utah Scientific Immunization Advisory Committee President-elect of Utah Chapter AAP Conflict of interest: None
Adolescent Immunizations While we do a pretty good job of immunizing our infants/toddlers: 4:3:1:3:3:1 USA 71.9% 4:3:1:3:3:1 Utah 74.9% 4:3:1:3:3:1 TriCounty 63.9%
Adolescent Immunizations • We don’t do as well protecting our teens: • Tdap: • USA 84.6% • Utah 81.5%
Pertussis • Utah outbreak: • 1544 cases in 2012 • 1219 cases in 2013 • Highest incidence age 12-16
Adolescent Immunizations • Meningococcal: • USA 74.0% • Utah 56.5% • TriCounty 32.7% • Rates of invasive meningococcal disease are estimated as about 1:100,000. However, each case has sudden devastating effects on an entire community.
Adolescent Immunizations • HPV 3 doses, Girls 13-17: • USA 33.4% • Utah 24.1% • TriCounty 5.5% • Boys ?
Human Papillomavirus • HPV is a cancer-causing virus. • We have an excellent, safe, effective vaccine. • We don’t use it to protect our teens. • Why?
HPV Infection • Almost all females and males will be infected with at least one type of HPV at some point in their lives • Estimated 79 million Americans currently infected • 14 million new infections/year in the US • HPV infection is most common in people in their teens and early 20s • Most people will never know that they have been infected Jemal A et al. J Natl Cancer Inst2013;105:175-201
HPV Infection • 80% of us have been (or will be) infected with HPV. • 2-5% of adults remain virgins. • Most will be exposed to HPV.
HPV Transmission • HPV exposure can occur with any type of intimate sexual contact • Intercourse is not necessary to become infected • Nearly 50% of high school students have already engaged in sexual (vaginal-penile) intercourse • 1/3 of 9th graders and 2/3 of 12th graders have engaged in sexual intercourse • 24% of high school seniors have had sexual intercourse with 4 or more partners Jemal A et al. J Natl Cancer Inst2013;105:175-201
HPV is found in virgins • Study examined the frequency of vaginal HPV and the association with non-coital sexual behavior in longitudinally followed cohort of adolescent women without prior vaginal intercourse • HPV was detected in 46% of women prior to first vaginal sex • 70% of these women reported non-coital behaviors that may in part explain genital transmission Shew, J Infect Dis. 2012
Rapid acquisition of HPV in following sexual debut Study of 18-23 year-old males (n=240)
Average Number of New HPV-Associated Cancers by Sex, in the United States, 2005-2009 n=1003 n=2317 n=3039 n=694 n=1687 n=3084 Oropharynx n=9312 n=11279 • Jemal A et al. J Natl Cancer Inst 2013;105:175-201
HPV-Associated Oropharyngeal Cancers • Prevalence increased from 16.3% (1984-89) to 71.7% (2000-04) • Population-level incidence of HPV-positive cancers increased by 225% while HPV-negative cancers declined by 50% If trends continue, the annual number of HPV-positive oropharyngeal cancers is expected to surpass the annual number of cervical cancers by the year 2020 Chaturvedi, 2011, J Clin Oncol- data from SEER
Why We Need to Do Better in HPV Vaccination of 12 year olds For each year we stay at 30% coverage instead of achieving 80%, 4,400 future cervical cancer cases and 1400 cervical cancer deaths will occur. • Currently 26 million girls <13 yo in the US; If none of these girls are vaccinated then: • 168,400 will develop cervical cancer and • 54,100 will die from it • Vaccinating 30% would prevent 45,500 of these cases and 14,600 deaths • Vaccinating 80% would prevent 98,800 cases and 31,700 deaths
Vaccines save lives (and anguish) • Most infected with HPV will have no symptoms. • Some feel shamed and disfigured by genital warts. • Some feel the fear and anguish of waiting for results of abnormal PAP smears or biopsies. • Some will experience cancer, hysterectomy, chemo, etc. • Some will die.
Guilt • All will have to deal with the burden of responsibility that they in turn also gave this virus to those they loved.
Alternatives to Vaccinating? • We can wait until the adolescent can safely make adult decisions…… • The pre-frontal cortex, responsible for emotional control and cognitive processing finally is fully formed by age 24-25. • We can hope that they “just say no”.
Sexual activity of teens • By age 12: 2% • By age 15 16% • By age 17 48% • By age 19 71% • http://www.guttmacher.org/pubs/FB-ATSRH.html
HPV Prophylactic Vaccines • Recombinant L1 capsid proteins that form “virus like” particles (VLP) • Non-infectious and non-oncogenic • Produce higher levels of neutralizing antibody than natural infection HPV VLP
HPV Vaccines • Gardisil covers HPV types 16, 18, and 6, 11 • Cervarix covers HPV types 16, 18 • Licenced for girls in 2006, for boys 2009
HPV Vaccine safety • 57 Million doses in the US • Safety similar to MCV4 and Tdap • Small risk of fainting
What can we do? • We cannot wait. • We must get our children protected while we can. The risk of exposure gets higher as months go by. • We, their health providers, must seize every opportunity to immunize our teens. A missed opportunity may well be our last (or only) chance.
Every teen • Identify needed vaccines for every teen that enters your office. • Teens have infrequent “well child” visits. • Sports exams, Scout exams. • Injury or illness visits. • Print vaccine forecast sheet for every teen (best for every child visit).
Delivery • This is a cancer vaccine. The conversation doesn’t have to be about sex. • We don’t spend a lot of time talking about the fecal-oral route, when we provide rotovirus vaccines. • Talking about modes of transmission just scares people off.
Delivery • If the parent asks about whether this vaccine is a license to take sexual risks, then site a study showing no increase in sexual activity after the vaccine. • http://pediatrics.aappublications.org/content/early/2012/10/10/peds.2012-1516
Delivery • HPV vaccine is no more a license to have sex, than the Tdap is license to go barefoot in the backyard and stomp around looking for nails.
Delivery • The strongest influence on whether a child gets the vaccines, is a strong recommendation from their doctor.
Delivery • After matter-of-factly announcing that of course their teen will get Tdap and Menactra, we (voice quavering) meekly suggest that we “need to talk” about HPV. Our delivery sends a louder message than our words. And our delivery is scaring some away.
Delivery • The message is: We can prevent these genital cancers….but only if we start now. Before exposure. • So, don’t be tentative. Deliver the message like somebody’s life depended on it.
HPV • The cancers are 20 years away. So why worry? • A time bomb, ticking down. And we don’t have a way to cut that red, no blue, wire. • But, we can prevent.
Teens • Teens, just like the toddlers they so recently were, are energetic, creative, and yet often obnoxious, • And they are worth saving.
Challenge • Go back to your office, and convince one family to immunize their teen. • Then, having saved a life (either this teen or one of their contacts)… • take the rest of the day off.